The Case
You get a call that a 50-year-old woman collapsed while running a marathon. Bystanders started CPR immediately. Nearby paramedics found her to be in ventricular fibrillation (VF). She was shocked three times and given 3 amps of epinephrine. She is still in VF when she arrives at your emergency department.
Explore This Issue
ACEP Now: Vol 36 – No 07 – July 2017Advanced cardiac life support (ACLS) was originally designed to give us a common language and help us avoid paralysis in a crisis situation. However, with each year that passes, it seems like ACLS has become more and more simplified to appeal to a broader scope of rescuers, including those who rarely run codes. Yet cardiac arrest physiology just isn’t that simple. Managing these patients requires a lot more finesse. Practitioners working in settings where they manage codes regularly (eg, the emergency department) should be expected to have a more sophisticated approach when standard ACLS algorithms aren’t effective. In this month’s column, I’ll suggest four strategies to improve the chances of return of spontaneous circulation (ROSC) in shock-resistant VF and, perhaps, survival to hospital discharge. Shock-resistant VF, or electrical storm, is defined as three or more sustained episodes of VF in a 24-hour period.
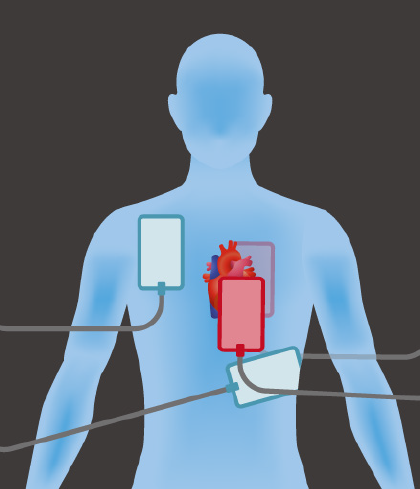
To perform dual-shock defibrillation, place one set of defibrillator pads in the traditional positions on the chest (blue pads) and attach a second set of pads from a second defibrillator in the anterior-posterior “sandwich” position (red pads).
ILLUSTRATION: Chris Whissen & Shutterstock.com
1. Prepare Your Team
Team-based preparation prior to patient arrival is essential to optimizing cardiac arrest care and takes fewer than five minutes. It can be broken down into three points to be discussed in a team huddle:
- What do we know? What do we expect to see? What are the possibilities? Run through the most likely immediate life-threatening issues.
- What do we do? What actions will you take, and what contingency plans will you have in place if those actions fail? Teams respond more efficiently and decidedly if they have anticipated failure rather than having failure of a plan surprise them.
- Role assignment: Assign logistical tasks to team members, including definitive airway management, chest compressions, medication administration, and defibrillation.
In this case, consider premixing amiodarone 300 mg and esmolol 500 mcg/kg and setting up for dual-shock therapy.
2. Consider Stopping Epinephrine
Epinephrine is associated with increased myocardial oxygen consumption and ventricular dysrhythmias and has never been shown to improve survival to hospital discharge in cardiac arrest.1 Epinephrine, in the doses used in cardiac arrest, causes cerebral vasoconstriction that may impair tissue oxygenation and brain perfusion and compromise neurological recovery.2 There is an argument to be made that epinephrine should be decreased or eliminated in all patients with shock-refractory VF because of its catecholamine effects. It makes little physiologic sense to add catecholamine fuel, like epinephrine, to the catecholamine firestorm of refractory VF. In fact, we want to achieve the opposite: Block the catecholamine surge so that the VF breaks.
3. Block Sympathetic Tone
Shock-resistant VF increases sympathetic tone, which leads to a vicious cycle of fibrillation and increased sympathetic tone.3 Esmolol decreases sympathetic tone and counteracts the endogenous and exogenous catecholamine surge theorized to occur during refractory VF arrest. Esmolol is the only drug in the management of cardiac arrest that has shown an increased rate of survival to hospital discharge with favorable neurologic outcomes. Albeit in a small study, patients who received esmolol after three defibrillations and 3 mg of epinephrine had a 50 percent survival to hospital discharge with a favorable neurologic outcome compared to 11 percent of patients who did not receive esmolol.4 Larger randomized controlled trials are needed. However, in the meantime, there is little downside to giving esmolol in this setting.
If you have the point-of-care ultrasound skills necessary, a second method to block sympathetic tone is to administer a stellate ganglion block.5 Case studies and one small randomized trial suggest reduced mortality in refractory VF with this method. The stellate ganglion at the level of C7 conducts sympathetic activity to the heart.
Directly blocking sympathetic outflow to the heart may decrease the sensitivity of the myocardium to arrhythmias.6
4. Consider Dual-Shock Defibrillation
If standard defibrillation isn’t working, consider double defibrillation. Animal studies show that most failed shocks are actually successful shocks but that the patient goes back into VF in less than one second. Eighty percent of patients who are resistant to a single shock will respond to dual shock.7 The idea is that you need to depolarize 90 percent of the myocardium to achieve effective defibrillation. If the patient has defibrillator pads in the traditional positions on the chest, attach a second set of pads from a second defibrillator in the anterior-posterior “sandwich” position (see image). At the time of defibrillation, both shock buttons are depressed simultaneously.
Adding a second set of pads changes the energy vectors through the myocardium, which helps achieve that 90 percent threshold. A few small studies have shown promising results for ROSC, with one showing 70 percent conversion with dual shock and 30 percent achieving ROSC in the field.8 It is important to note that the largest study to date on dual defibrillation in refractory VF did not show any benefit for neurologically intact survival.7
Don’t forget that since many patients with shock-resistant VF have an underlying cardiac ischemic event as the primary cause, cardiac arrest experts recommend consulting an interventional cardiologist for consideration of immediate transfer to the cath lab for all VF patients who have achieved ROSC.
Thanks to Jordan Chenkin, Paul Dorian, Laurie Morrison, and Steve Lin for their contributions to the podcasts that inspired this article.
 Dr. Helman is an emergency physician at North York General Hospital in Toronto. He is an assistant professor at the University of Toronto, Division of Emergency Medicine, and the education innovation lead at the Schwartz/Reisman Emergency Medicine Institute. He is the founder and host of Emergency Medicine Cases podcast and website (www.emergencymedicinecases.com).
Dr. Helman is an emergency physician at North York General Hospital in Toronto. He is an assistant professor at the University of Toronto, Division of Emergency Medicine, and the education innovation lead at the Schwartz/Reisman Emergency Medicine Institute. He is the founder and host of Emergency Medicine Cases podcast and website (www.emergencymedicinecases.com).
References
- Tang W, Weil MH, Sun S, et al. Epinephrine increases the severity of postresuscitation myocardial dysfunction. Circulation. 1995;92(10):3089-3093.
- Ristagno G, Tang W, Huang L, et al. Epinephrine reduces cerebral perfusion during cardiopulmonary resuscitation. Crit Care Med. 2009;37(4):1408-1415.
- Gao D, Sapp JL. Electrical storm: definitions, clinical importance, and treatment. Curr Opin Cardiol. 2013;28(1):72-79.
- Driver BE, Debaly G, Plummer DW, et al. Use of esmolol after failure of standard cardiopulmonary resuscitation to treat patients with refractory ventricular fibrillation. Resuscitation. 2014;85(10):1337-1341.
- Gadhinglajkar S, Sreedhar R, Unnikrishnan M, et al. Electrical storm: role of stellate ganglion blockade and anesthetic implications of left cardiac sympathetic denervation. Indian J Anaesth. 2013;57(4):397-400.
- Nademanee K, Taylor R, Bailey WE, et al. Treating electrical storm: sympathetic blockade versus advanced cardiac life support-guided therapy. Circulation. 2000;102(7):742-747.
- Ross EM, Redman TT, Harper SA, et al. Dual defibrillation in out-of-hospital cardiac arrest: a retrospective cohort analysis. Resuscitation. 2016;106:14-17.
- Hoch DH, Batsford WP, Greenberg SM, et al. Double sequential external shocks for refractory ventricular fibrillation. J Am Coll Cardiol. 1994;23(5):1141-1145.
Pages: 1 2 3 | Multi-Page





No Responses to “Treatment Strategies for Shock-Resistant Ventricular Fibrillation”