
Six accepted ED practices that are potentially harmful, costly, inefficient, or just don’t work
I’m always a bit tickled (yes, I said tickled) by the lofty discussions about evidenced-based medicine when much of what is done in medicine and many things we do in emergency medicine have little supporting evidence. It seems that our focus is the evolution of current management and diagnostic strategies and developing research strategies to prove or disprove our hypotheses. Although asking new questions and adding new literature to the world’s research database is critical to the evolution of medical practice, what is easier and more critical is questioning what we already do based on evidence that already exists. In other words, we might be asking the right question at the wrong time—or the wrong question altogether.
Explore This Issue
ACEP Now: Vol 33 – No 01 – January 2014As much as we claim to be scientists and practice with evidence as our guide, much of the care that is delivered in emergency departments comes from folklore. We have all—present company included—practiced in ways we absolutely believed to be best practice only to find out later that we may have been wrong. Hey, you don’t know what you don’t know.
There is great value in learning from great educators. However, we can get lost in the “greatness” of our mentors. Many edicts in medical education were taught to those we trust today by those whom they trusted yesterday. Once a learned, respected colleague states a “fact” with confidence, it often becomes unchallenged evidence and is passed down from one generation to the next. Evidence of my lack of social life, I enjoy using the “hot-tub time machine,” revisiting the land of lost medical questions to see if today’s evidence still supports these previously “answered” questions. It is amazing what you can find when you look.
Ultimately, there is still great latitude to practice the art of medicine. However, my goal is to challenge many commonly accepted practices that are potentially harmful, are expensive, create operational inefficiency, or simply just don’t work.
Prasad et al. published a very interesting article in JAMA in January 2012.1 They reviewed 35 clinical trials published in 2009 that tested established practices. They found that 46 percent of them contradicted current practice. This is evidence that medical reversals are common. Below are six myths worth challenging.
Many edicts in medical education were taught to those we trust today by those whom they trusted yesterday. Once a learned, respected colleague states a “fact” with confidence, it often becomes unchallenged evidence.
1. Tramadol or Tramacrap?
I’m no marketing expert, but despite that the name “Tramacrap” or “Ultracrap” would describe this drug perfectly, I doubt we’ll see a name change any time soon. Medve et al. published an article 12 years ago that demonstrates this nicely.2 They assessed the efficacy of tramadol for the treatment of dental pain, and in the emergency department, this indication is perfectly matched with the drug. Many physicians look for that “tweener” drug that the patient is less familiar with, is not an opioid, and still provides reasonable analgesia. This study identified the following order of efficacy (at eight hours): ibuprofen 400mg, tramadol/APAP 75/650, APAP 650, tramadol 75, and placebo. Further, the onset of action was 17 minutes for tramadol/APAP, 18 minutes for APAP, 34 minutes for ibuprofen, 51 minutes for tramadol, and 66 minutes for placebo.2 Tramadol does not taste great, nor is it less filling.
In addition, this drug does not play well with others. It is known to cause nausea and vomiting and confusion in the elderly, plus it has addictive potential (often referred to as a weak opiate),and creates a nasty overdose picture complicated by grand mal seizures.
2. “Banana Bags”
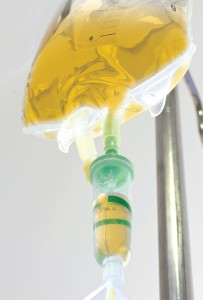 This is an expensive practice with little to no return on investment. Although everyone loves to see that yellow hydration solution pumping into the veins of the acutely intoxicated patient, what good are you really achieving? First, what is broken that you are fixing? Many of us have been taught that we must nutritionally replete intoxicated patients with multivitamins, thiamine, folic acid, and perhaps even B12. Even if you believe there is something to be fixed here, let’s think this through. How many of us are doing dietary counseling and securing a promise that our patients will eat better and take a daily vitamin before spending the time and money to acutely correct vitamin deficiencies in our intoxicated patients? In other words, if behavior isn’t modified, your good intentions are an expensive exercise in futility. More important, we are tilting at drunken windmills. These deficiencies don’t routinely exist. In 2008, Li et al. published an article assessing 75 acutely intoxicated patients for vitamin deficiencies (B12, folate, and thiamine).3 None of the patients had B12 or folate deficiencies, and only 15 percent had thiamine deficiencies (unknown clinical importance).
This is an expensive practice with little to no return on investment. Although everyone loves to see that yellow hydration solution pumping into the veins of the acutely intoxicated patient, what good are you really achieving? First, what is broken that you are fixing? Many of us have been taught that we must nutritionally replete intoxicated patients with multivitamins, thiamine, folic acid, and perhaps even B12. Even if you believe there is something to be fixed here, let’s think this through. How many of us are doing dietary counseling and securing a promise that our patients will eat better and take a daily vitamin before spending the time and money to acutely correct vitamin deficiencies in our intoxicated patients? In other words, if behavior isn’t modified, your good intentions are an expensive exercise in futility. More important, we are tilting at drunken windmills. These deficiencies don’t routinely exist. In 2008, Li et al. published an article assessing 75 acutely intoxicated patients for vitamin deficiencies (B12, folate, and thiamine).3 None of the patients had B12 or folate deficiencies, and only 15 percent had thiamine deficiencies (unknown clinical importance).
Hydration is important, but the routine use of multivitamins, thiamine, folic acid, and B12 are not.
3. Glucagon (Gluca-Gone) and Esophageal Obstructions
Although many patients will eventually resolve their food bolus obstructions spontaneously, they will still need a non-emergent EGD. Likewise, patients who don’t clear them need intervention and, at some point, an EGD. Why not make that point right now? Diagnostic or therapeutic, an urgent/emergent EGD is the most effective treatment. Are other treatments as effective as EGD for these obstructions? No. Let’s make glucagon “gluca-gone.” Leopard (a spotted surgeon from the United Kingdom) et al. published a systematic review of this topic in 2011.4 Hyoscine butylbromide was determined to be ineffective. Gas producers (eg, carbonated beverages) worked in 70 percent of cases, but glucagon was no better than placebo (one randomized, controlled trial and two other studies). However, EGD was effective in 93 percent to 100 percent of patients and found pathology in 55 percent to 90 percent of those cases.
4. Cardiac Enzymes and Syncope
Stop the madness. If the patient has had an AMI resulting in syncope, the history and/or ECG will have already told you. Routinely ordering cardiac enzymes solely for the chief complaint of syncope is a no-yield proposition. Two articles, from 2002 and 2003, respectively, address this issue. The first, in the Annals of Emergence Medicine, reviewed 741 AMI patients.5 Only 4 percent had a chief complaint of syncope. Even more compelling is the second article, where 2.1 percent of elderly patients presenting to the emergency department for syncope had positive enzymes. However, 100 percent of them had chest pain and ECG changes.6
5. Dilution (Delusional) Anemia
Is it physiologically true that when you administer intravenous fluids, the patient can suffer a dilutional anemia, or is this concept delusional? Yes, it is true, but this is a transient physiological phenomenon with very questionable clinical significance. In an article from 1996, euvolemic patients were enrolled in one of three arms: no IV fluids, maintenance IV fluids, and bolus IV fluids.7 Their blood counts were measured at one, four, and eight hours. The only group showing a difference was the bolus group at one hour. The reduction in hemoglobin and hematocrit were 1.5 and 4.1, respectively. This had resolved by four hours. In an additional study from 1989, it was proved that in healthy individuals who received volume infusions of normal saline equaling 46% of their blood volume, hematocrit dropped by 6% but quickly returned to normal and 60% of the infused volume diffused out of the intravascular space within 20 minutes.8
6. Cephalosporins and Penicillin Allergies
Put your worries and fears behind you. The chances of your penicillin-allergic patient actually having a reaction to a cephalosporin are very low. As a matter of fact, the likelihood that a patient reporting a penicillin allergy is actually allergic to penicillin is probably much lower than you may think. Even if the patient is allergic to penicillin, cross-reactivity is unlikely. In a systematic review of 27 articles by Johns Hopkins University and the University of Maryland, the authors reported that less than 10 percent of patients reporting allergies to penicillin actually had such an allergy.9 The rate of penicillin-related anaphylaxis ranged from 0.004% to 0.015%. Cross-reactivity for patients reporting penicillin allergy was 1% compared with 2.55% in those with proven allergies to penicillin. The structural link between cephalosporins and penicillin is the R1 side chain. Third- and fourth-generation cephalosporins do not have the R1 side chain and thus pose no risk. The first- and second-generation cephalosporins may possess the side chain. It is recommended to avoid the following first- and second-generation agents: cefadroxil, cefatrizine, cephalexin cephradine, cefaclor (2nd), and cefprozil (2nd).
Kevin M. Klauer, DO, EJD, FACEP is director of the Center for Emergency Medical Education (CEME) and chief medical officer for Emergency Medicine Physicians, Ltd., Canton, Ohio; on the Board of Directors for Physicians Specialty Limited Risk Retention Group; assistant clinical professor at Michigan State University College of Osteopathic Medicine; and medical editor in chief of ACEP Now.
References
- Prasad V, Cifu A, Ioannidis JP. Reversals of established medical practices: evidence to abandon ship. JAMA. 2012;307:37-38.
- Medve RA, Wang J, Karim R. Tramadol and acetaminophen tablets for dental pain. Anesth Prog. 2001;48:79-81.
- Li SF, Jacob J, Feng J, et al. Vitamin deficiencies in acutely intoxicated patients in the ED. Am J Emerg Med. 2008;26:792-795.
- Leopard D, Fishpool S, Winter S. The management of oesophageal soft food bolus obstruction: a systematic review. Ann R Coll Surg Engl. 2011;93:441-444.
- Gupta M, Tabas JA, Kohn MA. Presenting complaint among patients with myocardial infarction who present to an urban, public hospital emergency department. Ann Emerg Med. 2002;40:180-186.
- Grossman SA, Van Epp S, Arnold R, et al. The value of cardiac enzymes in elderly patients presenting to the emergency department with syncope. J Gerontol A Biol Sci Med Sci. 2003;58:1055-1058.
- Grathwohl KW, Bruns BJ, LeBrun CJ, et al. Does hemodilution exist? Effects of saline infusion on hematologic parameters in euvolemic subjects. South Med J. 1996;89:51-55.
- Greenfield RH, Bessen HA, Henneman PL. Effect of crystalloid infusion on hematocrit and intravascular volume in healthy, nonbleeding subjects. Ann Emerg Med. 1989;18:51-55.
- Campagna JD, Bond MC, Schabelman E, et al. The use of cephalosporins in penicillin-allergic patients: a literature review. J Emerg Med. 2012;42:612-620.
Pages: 1 2 3 | Multi-Page





3 Responses to “Myths in Emergency Medicine”
March 20, 2014
tramadol efficacy? | DAILYEM[…] article by Dr. Klauer in January’s ACEP Now. covers a few topics, but here’s one […]
December 19, 2014
Myths in Emergency Medicine | VGH Emergency Department[…] https://www.acepnow.com/article/myths-emergency-medicine/ […]
January 10, 2019
MegWhere are your links to sources?