The Case
A 52-year-old woman presents to the emergency department with sudden onset of palpitations and presyncope starting one hour ago. There has been no chest pain or shortness of breath. Examination is normal other than an irregularly irregular heart rate of 150 beats per minute. The patient’s past medical history is significant for gastroesophageal reflex disease for which she takes a proton pump inhibitor. The ECG shows classic atrial fibrillation with a rapid ventricular response.
Explore This Issue
ACEP Now: Vol 38 – No 11 – November 2019Background
Atrial fibrillation is the most common significant dysrhythmia in the emergency department.1 For decades, experts have debated whether a rhythm control or rate control strategy is best (eg, RAte Control versus Electrical cardioversion for atrial fibrillation [RACE] and Atrial Fibrillation Follow-up Investigation of Rhythm Management [AFFIRM]).2,3 The American College of Cardiology/American Heart Association/Heart Rhythm Society 2014 guidelines contain recommendations on the management of patients with atrial fibrillation.4
Practice variation in management of patients with atrial fibrillation has been noted. Physicians in the United Kingdom and Australia use rhythm control approximately half the time, while American physicians employ rhythm control one-quarter of the time.5
In Canada, the proportion undergoing rhythm control ranges from 42 to 85 percent. Even once rhythm control is selected, practice management varies. A chemical-first rhythm control approach is used in 56 percent of patients, while an electrical-first approach is used in 44 percent of patients.6
Clinical Question
In patients with acute uncomplicated atrial fibrillation, is sinus rhythm achieved faster with chemical-first or electrical-first rhythm control?
Reference: Scheuermeyer FX, Andolfatto G, Christenson J, et al. A multicenter randomized trial to evaluate a chemical-first or electrical-first cardioversion strategy for patients with uncomplicated acute atrial fibrillation. Acad Emerg Med. 2019;26(9):969-981.
- Population: Patients ages 18 to 75 years with atrial fibrillation of less than 48 hours duration with a CHADS2 score <2 (see Table 1).
- Excluded: Hemodynamic instability, atrial flutter, CHADS2 score ≥2, acute underlying medical illness, recent cardiac procedure, acute intoxication, or withdrawal from alcohol or illicit substances. Other excluded patients included those who came to the emergency department for other reasons (eg, trauma, gout) who were incidentally found to have atrial fibrillation.
- Intervention: Chemical-first rhythm control using IV procainamide followed by electrical cardioversion (if chemical cardioversion was unsuccessful).
- Comparison: Electrical-first rhythm control using a synchronized biphasic waveform sequence of 100J to 150J to 200J, with a maximum of three attempts, followed by chemical cardioversion with procainamide (if electrical cardioversion was unsuccessful).
- Outcome:
- Primary Outcome: Discharge within four hours of ED arrival.
- Secondary Outcomes: Additional median time intervals, ED-based adverse events, and 30-day patient-centered outcomes.
Authors’ Conclusions
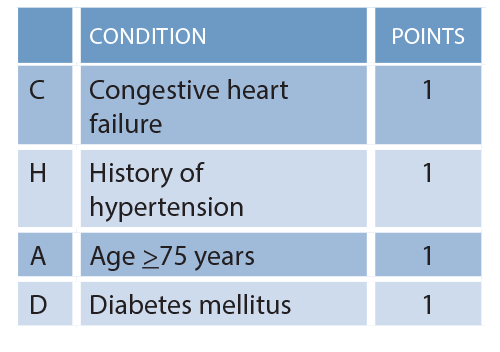
Table 1: CHADS2 Calculation
“In uncomplicated ED [atrial fibrillation] patients, chemical-first and electrical-first strategies both appear to be successful and well tolerated; however, an electrical-first strategy results in a significantly shorter ED length of stay. Our results should encourage clinicians to initially consider an electrical-first approach for such patients.”
Key Results
Eighty-four patients were enrolled. The median age was in the late 50s. More than a third of patients were female, and three-quarters had a history of atrial fibrillation.
- Primary Outcome: Patients discharged in less than four hours of ED arrival.
- 32 percent chemical cardioversion first versus 67 percent electrical cardioversion first
- 36 percent difference (95 percent CI, 16–56 percent; P<0.001), number needed to treat=3.
- Secondary Outcomes:
- Median time in the emergency department: 5.1 hours chemical cardioversion first versus 3.5 hours electrical cardioversion first.
- Adverse events: 24 percent chemical cardioversion first versus 26 percent electrical cardioversion first. Both groups had minimal risk outcomes. There were no strokes or deaths in either group at 30 days.
- Quality-of-life scores: Similar at 3 and 30 days for both groups across all domains.
Evidence-Based Medicine Commentary
- Consecutive Patients: Recruitment depended on whether a research assistant was available. This could have introduced selection bias into the study.
- Exclusion: Patients over the age of 75 were excluded. This could limit the application of these data to older patients who present with atrial fibrillation.
- Outcome: The primary outcome was changed from ED length of stay to a dichotomous outcome of the proportion of patients discharged within less than four hours of ED arrival. The changing of a primary outcome during a trial can be problematic and has been described in the literature.7 However, in this manuscript, the authors explained that the change was made to ensure a straightforward sample size calculation.
- Tertiary and community: This study included sites ranging from large tertiary referral centers to smaller community hospitals without the availability of on-site cardiologists. This strengthens the validity of the results.
- External validity: This study was conducted in six urban Canadian emergency departments. It may not have external validity to other countries like the United States, Australia, and the United Kingdom where different approaches to similar patients may be in common use.
Bottom Line
An electrical-first rhythm control cardioversion strategy for acute uncomplicated patients with atrial fibrillation can shorten ED lengths of stay.
Case Resolution
A shared decision is made to use an electrical-first rhythm control cardioversion strategy.
Thank you to Dr. Chris Bond, clinical lecturer at University of Calgary in Alberta, for his help with this review.
Remember to be skeptical of anything you learn, even if you heard it on the Skeptics’ Guide to Emergency Medicine.
References
- Naccarelli GV, Varker H, Lin J, et al. Increasing prevalence of atrial fibrillation and flutter in the United States. Am J Cardiol. 2009;104(11):1534-1539.
- Van Gelder IC, Hagens VE, Bosker HA, et al. A comparison of rate control and rhythm control in patients with recurrent persistent atrial fibrillation. N Engl J Med. 2002;347(23):1834-1840.
- Wyse DG, Waldo AL, DiMarco JP, et al. A comparison of rate control and rhythm control in patients with atrial fibrillation. N Engl J Med. 2002;347(23):1825-1833.
- January CT, Wann LS, Alpert JS, et al. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2014;64(21):e1-76.
- Decker WW, Smars PA, Vaidyanathan L, et al. A prospective, randomized trial of an emergency department observation unit for acute onset atrial fibrillation. Ann Emerg Med. 2008;52(4):322-328.
- Stiell IG, Clement CM, Brison RJ, et al. Variation in management of recent-onset atrial fibrillation and flutter among academic hospital emergency departments. Ann Emerg Med. 2011;57(1):13-21.
- Ramagopalan S, Skingsley AP, Handunnetthi L, et al. Prevalence of primary outcome changes in clinical trials registered on ClinicalTrials.gov: a cross-sectional study. F1000Res. 2014;3:77.
Pages: 1 2 3 | Multi-Page





No Responses to “In Uncomplicated AFib, Is Electrical or Chemical Rhythm Control Best?”