Use of regional anesthesia is becoming more prevalent in the emergency department as more data emerge about its safety, efficacy, and, in many cases, associated decreased length of stay. Procedural sedation requires intravenous access, dedicated personnel for both the sedation and procedure, and a room within the emergency department equipped to provide airway management and resuscitation in the event of complications from IV anesthesia. Complications include hypoventilation/apnea, aspiration, laryngospasm, and hypotension. Often, the required painful procedure is brief, but the discomfort associated with the illness is long-lasting; procedural sedation provides anesthesia for a brief period of time, but does not control pain after the sedation is over. Regional anesthesia provides pain relief lasting for hours, allowing intervention in the patient’s acute illness without subjecting him or her to the risks of sedation. For patients whose injuries require transfer to a center with broader expertise, regional anesthesia can provide critical pain control without a change in respiratory pattern or mental status that could become dangerous during transit.
In the emergency department, ultrasound-guided brachial plexus block can provide rapid and definitive pain relief from traumatic injuries to the upper extremity. Emergency physicians have published data on using two approaches (interscalene and supraclavicular) for the ultrasound-guided brachial plexus block.1,2 Either can be used as a primary or supplementary method to provide analgesia for traumatic injuries and infections, including humeral fractures, upper-extremity joint reduction, abscess drainage, and burns. The interscalene and supraclavicular brachial plexus blocks are considered ultrasound-guided procedures with intermediate difficulty. However, the interscalene approach allows for identification of the brachial plexus while maintaining a greater distance from vascular structures and pleura than the supraclavicular approach. A simplified method to locate and perform the block will allow for integration of this useful procedure into the practice of emergency medicine. Both blocks are performed with ultrasound guidance in the emergency department setting. While anesthesiologists may use nerve stimulators to achieve these blocks, this technique is not typically employed in the emergency department. Moreover, there is evidence suggesting that ultrasound provides superior efficacy, compared with nerve stimulator block of the brachial plexus at the interscalene level.3
Clinical Indications
The ultrasound-guided interscalene brachial plexus block provides regional anesthesia to the entire upper extremity including the shoulder. Anesthesiologists routinely utilize the interscalene brachial plexus block during orthopedic surgery to provide anesthesia to the lateral clavicle, acromioclavicular joint, proximal humerus, and elbow. In the emergency department, current indications for the interscalene block include pain control for upper-extremity fractures (proximal humerus, midshaft humerus, etc.) and to facilitate manipulations and reductions of upper-extremity injuries. Also, the interscalene brachial plexus block may be an ideal alternative in the setting of large abscess incision and drainage, deep wound exploration, and complex laceration repair when procedural sedation is not feasible.
Although the interscalene approach has a lower risk of iatrogenic pneumothorax than the supraclavicular approach secondary to the higher approach on the neck, it is more likely to cause phrenic nerve paralysis due to tracking of local anesthetic around the anterior scalene muscle. Traditional high volumes injections of local anesthetic (greater than 30 mL) will reliably affect the phrenic nerve and cause paralysis of the ipsilateral hemidiaphragm for the duration of the block.4 While clinically insignificant in healthy patients, the risk of phrenic nerve paralysis may potentially be decreased by using small-volume intraplexus injections under real-time ultrasound guidance.5 However, since currently there is no clear evidence suggesting that phrenic nerve paralysis can be reliably avoided, this block is not recommended for patients with known low pulmonary reserve such as those with chronic obstructive pulmonary disease.
Furthermore, it is not recommended that the block be used in patients who are intoxicated, demented, or otherwise without normal mental status, as the patient’s report of paresthesias, worsening pain, or other symptoms during the procedure helps avoid complications from misdirected anesthetic (intravascular or intraneural injection). Also, postblock evaluation for peripheral nerve injury (PNI) will not be possible if a consistent neurologic exam cannot be performed before the procedure is started.
Anatomy
The brachial plexus originates from the anterior rami of the C5-T1 spinal nerves and divides into the roots, trunks, divisions, and cords that ultimately contribute to the axillary, radial, median, and ulnar nerves that provide cutaneous and motor innervation for the entire upper limb. After exiting the neural foramina, the brachial plexus travels through the interscalene groove between the anterior and middle scalene muscles and joins the subclavian artery anterior to the first rib and posterior to the clavicle. This neurovascular bundle travels to the axilla and supplies both motor and sensory innervation to the entire upper extremity via the axillary, musculocutaneous, radial, median, and ulnar nerves. When successfully performed, the interscalene block may also affect the distal branches of the divisions and cords that give rise to the suprascapular, lateral and medial pectoral, thoracodorsal, and subscapular nerves.
The interscalene approach targets the brachial plexus at the level of the roots or trunks as they pass lateral to the great vessels and through the interscalene groove between the anterior and medial scalene muscles. The interscalene groove is located deep to the clavicular head of the sternocleidomastoid muscle and is bordered medially by the anterior scalene muscle and laterally by the middle scalene. Important landmarks that lie medial to the anterior scalene muscle include the carotid artery, internal jugular vein, and phrenic nerve. The dome of the pleura is located caudad and should not be considered at risk if the block is performed correctly at the level of the larynx.
Occasionally, the interscalene block will fail to anesthetize the C8 dermatome that provides sensation to the fifth digit and distal medial forearm. This is because of a described anatomic variation in which the C8 nerve root lies deep to the C5-7 plexus and is separated by an additional fascial layer or muscle bridge that may limit the spread of local anesthetic.6 For emergency physicians who are using this block for proximal upper-extremity injuries, the lack of complete anesthesia of the C8 root is not clinically significant. For patients who require complete anesthesia below the elbow, a supraclavicular or infraclavicular approach may be more desirable.
The Procedure: Ultrasound-Guided Interscalene Brachial Plexus Nerve Blocks Patient Positioning and Probe Selection
The patient is placed on a cardiac monitor and positioned supine in a semireclining position with the head rotated 30 degrees away from the side of the injury. The ultrasound screen and cardiac monitor should be directly opposite the patient so that the physician can easily view the display screen while performing the block, permitting the visualization of the neck and ultrasound screen in the same visual axis (Fig. 1). A high-frequency linear transducer probe with a large footprint is ideal for the procedure. Always clean the ultrasound probe in a standard fashion and place a clear adherent dressing over the probe (Fig. 2), using sterile surgical lubricant as a coupling agent.
Choice of Local Anesthetic
Lidocaine 1%-2% drawn into a 20- to 30-mL syringe is recommended. All providers using nerve blocks should be familiar with the standard recommended dosages and clinical signs of toxicity, and have established protocols for treatment of local anesthetic toxicity that incorporate use of lipid infusions. For novice users, lidocaine rather than bupivacaine is recommended because of its better safety profile in cases of inadvertent vascular injection. Using epinephrine-containing anesthetics can prolong the duration of the block, and also provides an additional safety benefit: Sudden tachycardia, hypertension, and characteristic electrocardiographic T-wave morphology changes indicate accidental intravascular injection, alerting providers before large volumes of local anesthetics have been injected. A standard 21- to 23-gauge, 1.5-inch needle provides adequate visualization without significant tissue trauma but may not have sufficient length to reach the interscalene groove. For this reason, a 3.5-inch spinal needle is recommended in cases in which the depth of the relevant structures appears significantly deep to the skin surface as it interfaces with the ultrasound probe (Fig. 3).
Injection Technique
Place a high-frequency linear transducer in a transverse orientation (probe marker facing the right of the patient) at the level of the larynx, identifying the internal jugular vein (IJV) and carotid artery. Clinicians comfortable with ultrasound-guided cannulation of the IJV should be able to locate the vascular anatomy of the neck at this level. From this position, slowly move the probe laterally past the great vessels until the border of the clavicular head of the sternocleidomastoid muscle (SCM) comes into view midscreen (Fig. 4).
At this level, the anterior and middle scalene muscles lie just deep to the SCM, with the interscalene groove located between the two prominent muscles. The nerve roots of the brachial plexus will be visualized as oval or round hypoechoic structures located in the groove between the anterior and middle scalene muscles, where they are tightly clustered within their own fascial sheath. Here the C5-7 roots of the brachial plexus appear as three vertically aligned, round hypoechoic structures, sometimes referred to as the “traffic light” sign (Fig. 5).
The C8 root may be located within this fascial plane or may be deeper as previously mentioned. Lateral to the brachial plexus is the middle scalene muscle, comprising the lateral border of the interscalene groove. The transverse cervical and suprascapular arteries typically run laterally and caudad to the brachial plexus at this level. After the brachial plexus is located, color Doppler is recommended to confirm that vasculature structures will not be present in the path of the needle and/or mistaken for hypoechoic nerve roots.
An alternative approach to finding the brachial plexus (if the provider is having difficulty locating the structures at the level of the larynx) involves identifying the brachial plexus distally at the level of the supraclavicular fossa and following the nerve trunks proximally into the interscalene groove. Here, the transducer is placed transversely in the supraclavicular fossa and aimed caudally until the subclavian artery is visualized. The brachial plexus lies just posterolateral to the artery at this level and will appear as a tight group, a hypoechoic “cluster of grapes.” Follow these hypoechoic structures cephalad until they form the traffic light sign within the interscalene groove at the level of the larynx (Fig. 6).
Needle Insertion and Injection
Two distinct injection techniques have been described:
- The classic periplexus approach targets the potential space between the middle scalene muscle and the brachial plexus sheath. This approach reduces the risk of intraneural injection but requires higher volumes of local anesthetic to achieve a complete block. Unfortunately, large volumes of anesthetic are thought to be more likely to track around the anterior scalene muscle to the phrenic nerve, causing paralysis of the ipsilateral hemidiaphragm.
- The intraplexus approach targets the space between the nerve roots within the brachial plexus sheath and requires smaller volumes of local anesthesia to achieve an adequate block. Lower volumes of injected anesthetic limits spread to the phrenic nerve but may also result in anesthetic tracking superiorly within the plexus sheath, affecting the recurrent laryngeal nerve and/or sympathetic chain, causing temporary hoarseness or Horner’s syndrome, respectively.
The authors recommend performing the interscalene brachial plexus with an in-plane technique so that the needle is visualized in its entirety. After cleaning the skin with a sterilizing solution such as chlorhexidine, and covering the cleaned ultrasound probe with a sterile adhesive dressing, place 2-3 mL of lidocaine (with or without epinephrine) about 0.5-1 cm lateral to the ultrasound probe. This will be the location of entry for the block needle, and adequate local anesthesia will allow for patient comfort during the block.
Enter the skin at the site of the local skin wheal in a lateral to medial in-plane approach. Flatter needle angles will allow for better needle visualization, which will depend on the depth and location of the brachial plexus. Advance the needle in 1- to 2-cm increments, maintaining clear visualization of the needle tip at all times. This block may be performed with either an in-plane or out-of-plane approach.
In many cases, the authors prefer an in-plane approach because the needle tip can be better visualized, allowing for more precise intraplexus injections. The needle is inserted lateral to the lateral aspect of the transducer. For a periplexus injection, the needle tip is advanced through the middle scalene muscle to the lateral border of the deepest nerve root. Local anesthetic (15-20 mL) is delivered into the potential space between the middle scalene muscle and the brachial plexus sheath (Fig. 7).
For an intraplexus injection, the needle is advanced into the brachial plexus sheath between the two most superficial nerve roots and a low-volume injection of 5-10 mL may be used. For all ultrasound-guided nerve blocks, frequent aspiration to confirm lack of vasculature puncture and visualization of the needle (including needle tip) are recommended before injection.
Finally, if anechoic fluid is not seen on the ultrasound screen (or if high injection pressures or parethesias are encountered) when injecting anesthetic, the procedure should be halted, and the visualization of the needle tip should be confirmed. Local anesthetic will track around the brachial plexus bundle, producing the classic “donut” sign.
Evaluating Block Efficacy
Successful blocks are associated with direct visualization of hypoechoic anesthetic adjacent to the brachial plexus in the interscalene groove, as well as fluid tracking in the fascial plane. Waiting at least 20 minutes before performing the motor and sensory exam of the upper extremity is recommended. Block duration should be approximately 1-3 hours, but a block occasionally lasts as long as 6 hours.
Aftercare
After the block is performed, the time and date of the block should be marked on the patient’s skin with a sterile marking pen (if they are being admitted) or noted in discharge paperwork. Patients should be reminded that they are at risk of injuring the affected extremity because of the anesthesia. A sling should be provided to support the arm even if not otherwise warranted by the injury. Patients should be given strict verbal and written instructions to return for persistent paresthesias, weakness, or severe pain that lasts more than 48-72 hours.
Summary
The interscalene approach to the brachial plexus block provides effective anesthesia for painful traumatic and infectious conditions of the upper extremity. Ultrasound guidance allows the emergency physician to perform this block safely. The interscalene brachial plexus is identified between the scalene muscles at the level of the larynx, or followed up from the supraclavicular location, where the plexus is more unified. Local anesthetic is delivered via the periplexus or intraplexus approach, with the needle visualized in-plane. The patient’s neurologic exam should be recorded before and after the block, and appropriate aftercare and return precautions given.
References
- Blaivas M, Adhikari S, Lander L. A prospective comparison of procedural sedation and ultrasound-guided interscalene nerve block for shoulder reduction in the emergency department. Acad. Emerg. Med. 2011;18(9):922-7.
- Stone MB, Wang R, Price DD. Ultrasound-guided supraclavicular brachial plexus nerve block vs procedural sedation for the treatment of upper extremity emergencies. Am. J. Emerg. Med. 2008;26(6):706-10.
- Kapral S, Greher M, Huber G, et al. Ultrasonographic guidance improves the success rate of interscalene brachial plexus blockade. Reg. Anesth. Pain Med. 2008;33(3):253-8.
- Urmey WF, Talts KH, Sharrock NE. One hundred percent incidence of hemidiaphragmatic paresis associated with interscalene brachial plexus anesthesia as diagnosed by ultrasonography. Anesth. Analg. 1991;72(4):498-503.
- Riazi S, Carmichael N, Awad I, Holtby RM, McCartney CJL. Effect of local anaesthetic volume (20 vs 5 ml) on the efficacy and respiratory consequences of ultrasound-guided interscalene brachial plexus block. Br. J. Anaesth. 2008;101(4):549-56.
- Marhofer P, Harrop-Griffiths W, Willschke H, Kirchmair L. Fifteen years of ultrasound guidance in regional anaesthesia, Part 2: Recent developments in block techniques. Br. J. Anaesth. 2010;104(6):673-83.



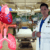

No Responses to “Ultrasound-Guided Interscalene Approach To the Brachial Plexus Nerve Block”