Editors’ Note: This article was accepted on June 28, 2020, and was accurate at that time. Because information about SARS-CoV-2 and COVID-19 is evolving rapidly, please verify these recommendations and information.
Explore This Issue
ACEP Now: Vol 39 – No 08 – August 2020COVID-19 has disproportionately affected various regions in the United States. One area, New York City, dominated the press with dramatic stories of death and heroism. Another, the Navajo Nation, spanning three states in the Southwest, received minimal national attention until recently, despite having higher per capita cases than any state. With approximately 350,000 inhabitants living within 27,000 square miles, the Navajo Nation has seen a dramatic increase since March to 3,740 positive COVID-19 cases and 127 deaths as of May 14.1 The Navajo Nation rate of infection was 10 times higher than that of the state of Arizona during this period.2
The Navajo Nation had been under-resourced and medically underserved long before this pandemic struck. Vulnerabilities include the Nation’s historical lack of resources and sufficient medical care, a high number of medical comorbidities among this susceptible population, a widespread lack of running water that makes frequent handwashing and proper hygiene difficult, and distributed governance. In addition, the Navajo tend to live communally, with multigenerational families in single-room homes. At the intersection of culture, governance, and health, COVID wreaked havoc.
Team Rubicon is a nongovernmental nonprofit disaster relief organization founded in 2010 that provides domestic disaster and international humanitarian response using the skills and experience of veterans. Team Rubicon volunteers have deployed across the country in response to the COVID-19 pandemic to assist with both medical and nonmedical services.

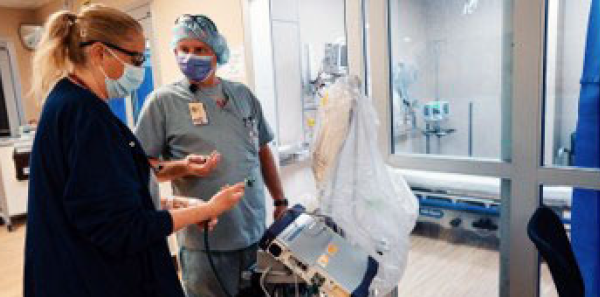
Dr. Chartoff at Kayenta Health Center.
Stanley Chartoff
In April 2020, we were part of a group that Team Rubicon deployed to Kayenta, Arizona, in an area of the Navajo Nation especially hard hit by COVID-19. Our mission was to provide assistance with medical and incident command personnel and supplies for the Kayenta Health Center and the surrounding region. Team Rubicon volunteers (known as Greyshirts) deployed to the area included incident command (IC) support staff as well as physicians, physician assistants, nurses, paramedics, and EMTs. These volunteers helped in the health center’s command center as well as the Kayenta Emergency Department and the Navajo EMS service, augmenting local staff stressed by the effects of the COVID-19 pandemic.
The Kayenta Health Center, a part of the Indian Health Service, was built in 2016 and has a 24-7 emergency department with 10 rooms, including a trauma room and a negative pressure room, as well as a pharmacy, a lab, and a radiology suite including a CT scanner. There are no inpatient facilities, necessitating transfers by ground, helicopter, or fixed-wing aircraft.
As in other areas, COVID-19 has resulted in a decrease in total volume but a dramatic increase in the acuity of patients seen at Kayenta Health Center. Since the start of the pandemic, the facility has shifted to disaster mode and created an incident command center to monitor and control the response. Access and movement within the facility is controlled to decrease the chance of spreading infection, and temperature checks are performed daily on everyone entering the building. Team Rubicon IC staff helps monitor and assure availability of personal protective equipment (PPE) and tracks staff exposures.
Both of us typically work in urban academic medical centers. Working in Kayenta, a rural critical-access emergency department, provided clinical, operational, and cultural challenges. But the experience also provided ample opportunities for humility.
Many elderly patients only speak Navajo, requiring staff to help with language translation. Most of the COVID patients we saw were extremely ill when they presented. It was not uncommon to see multiple patients from the same family, especially since those who were infected with coronavirus but not sick enough for admission would be discharged back to their communal homes—there were no facilities for them to self-quarantine. Patients who might be managed at home with prone positioning and high-flow nasal oxygen would require intubation to assure a safe airway during flight to accepting facilities, often as far away as Phoenix, about 300 miles away. Sometimes flights would be delayed, resulting in a need to manage a critically ill patient on a ventilator for a prolonged period, sometimes with limited equipment and medication supplies.
After SARS-CoV-2 began to afflict the Navajo Nation, the already-stressed medical system was strained far beyond its capabilities. The region in the center of the Nation has been leading the number of positive COVID cases with only an emergency department to care for their patients. Team Rubicon recognized the need for outside medical support early and asked for volunteers to deploy to the hardest-hit region of the Navajo Nation at Kayenta. Team Rubicon has been able to assist the medical mission as well as provide acutely needed PPE. The Indian Health Service staff has been grateful for the support as well as the critical care expertise and education Team Rubicon was able to provide.
The COVID-19 pandemic produced Team Rubicon’s first domestic medical responses, to the Navajo Nation as well as a federal medical station in Santa Clara, California, and a drive-through testing center in Charlotte, North Carolina. These missions illustrate how a nonprofit can work with governmental and private organizations to meet the needs during a pandemic disaster.
Dr. Bradley is a disaster/operational medicine and EMS fellow in the department of emergency medicine at Atrium Health-Carolinas Medical Center in Charlotte, North Carolina.
Dr. Chartoff is assistant professor of emergency medicine at the University of Connecticut School of Medicine in Hartford, an emergency physician at the University of Connecticut–Hartford Hospital, and medical director of Team Rubicon Northeast Territory.
References
- COVID-19. Navajo Department of Health website. Accessed July 31, 2020.
- Scher I. The Navajo Nation‘s coronavirus infection and death rates are 10 times higher than the neighboring state of Arizona. Business Insider. Apr 20, 2020. Accessed July 31, 2020.
Pages: 1 2 | Multi-Page

 The day had been very typical, with plenty presenting for COVID-19-related symptoms or mainly minor complaints. I sat there wondering when we would get our sick patient that day, as we had seemed to reach the point of averaging at least one COVID-19-infected patient per day who was critically ill enough to require intubation and transport. It wasn’t soon after that we were notified there was a critical patient being brought back with hypoxia and tachypnea and concern for COVID-19. The next thing we noticed was this was not one of our typical patients but one of our own emergency department teammates…
The day had been very typical, with plenty presenting for COVID-19-related symptoms or mainly minor complaints. I sat there wondering when we would get our sick patient that day, as we had seemed to reach the point of averaging at least one COVID-19-infected patient per day who was critically ill enough to require intubation and transport. It wasn’t soon after that we were notified there was a critical patient being brought back with hypoxia and tachypnea and concern for COVID-19. The next thing we noticed was this was not one of our typical patients but one of our own emergency department teammates… I was on duty for my first evening shift in the Kayenta emergency department when a patient who had previously tested positive for the novel coronavirus and was short of breath was being brought back in a wheelchair. I saw on the tracking board that she was 28 years old. One of the other physicians started donning his PPE in anticipation of treating her when she suddenly slid out of the wheelchair and collapsed on the floor in front of the nurse’s station…
I was on duty for my first evening shift in the Kayenta emergency department when a patient who had previously tested positive for the novel coronavirus and was short of breath was being brought back in a wheelchair. I saw on the tracking board that she was 28 years old. One of the other physicians started donning his PPE in anticipation of treating her when she suddenly slid out of the wheelchair and collapsed on the floor in front of the nurse’s station…



No Responses to “Team Rubicon Responds to COVID-19 Crisis in the Navajo Nation”