The best questions often stem from the inquisitive learner. As educators, we love, and are always humbled by, those moments when we get to say, “I don’t know.” For some of these questions, you may already know the answers. For others, you may never have thought to ask the question. For all, questions, comments, concerns, and critiques are encouraged. Welcome to the Kids Korner.
Explore This Issue
ACEP Now: Vol 36 – No 07 – July 2017Question 1: Are serum lactate levels good screening tools for sepsis in pediatric patients?
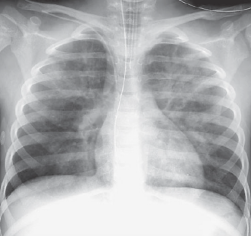
There is a patchy distribution of pulmonary edema
in this 6-year-old near-drowning patient.
PHOTO: Wells RG. Diagnostic Imaging of Infants and Children; 2015. © 2017 McGraw-Hill Education. All rights reserved. McGraw-Hill Education makes no representations or warranties as to the accuracy of any information related to this image. In no event shall McGraw-Hill Education have any liability to any party for special, incidental, tort, or consequential damages arising out of or in connection with it.
In adults, a screening serum lactate ≥4 mmol/L identifies patients at significantly higher risk of death from sepsis, serving as a valuable risk stratification tool.1 For this reason, it is common practice to obtain this test in adult patients suspected of having sepsis. However, in children, there are considerably less data on this topic.
The literature on this topic has typically been limited to pediatric ICU patients. One early study was a very small (n=11) prospective pediatric ICU study.2 The authors evaluated children ages 1 to 18 years in septic shock who required mechanical ventilation. In these 11 children, they drew 53 serum lactate samples—an initial sample in each, plus six-hour trending follow-up samples. In these patients, only 15 of 53 (29 percent) samples were >1.8 mmol/L. Of the initial lactates drawn, only 2 of 11 (18 percent) were >4 mmol/L, suggesting that serum lactates are not good screening tests for severe sepsis/septic shock in pediatric patients. Another retrospective study of 289 children younger than 18 years evaluated screening serum lactate measurements as an outcome predictor in a pediatric emergency department.3 Death was not predicted by the serum lactate in that study.
A later prospective observational cohort study (n=239) evaluated screening serum lactate levels in children younger than 19 years if they met systemic inflammatory response syndrome (SIRS) criteria.4 Predefined levels of serum lactates were normal (< 2 mmol/L), intermediate (2–4 mmol/L), and hyperlactatemia (>4 mmol/L). The primary endpoint was end-organ dysfunction within 24 hours. For patients with hyperlactatemia (>4 mmol/L), the sensitivity for end-organ dysfunction was only 31 percent (4 of 13); the majority of patients with end-organ damage within 24 hours of ED presentation presented in the <4 mmol/L group. While the relative risk of end-organ damage within 24 hours was higher (5.5; 95% CI,1.9–16) in the hyperlactatemia group, having a serum lactate <4 mmol/L did not rule out a seriously septic child, suggesting that practitioners should not use screening serum lactates alone to risk-stratify pediatric patients suspected of having sepsis.
A recent pediatric prospective, observational, cohort study (n=1,299), similar to previous adult studies, evaluated whether an elevated screening serum lactate >36 mg/dL (>4 mmol/L) was associated with increased mortality in pediatric patients.5 The primary outcome was in-hospital, all-cause mortality within 30 days. The overall mortality was 1.9 percent (25 of 1,299). In patients with lactates >36 mg/dL, the mortality was 4.8 percent (5 of 103) versus 1.7 percent (20 of 1,196) in the group <36 mg/dL. While the mortality in the hyperlactatemia group (>36 mg/dL) was higher, the difference in mortality was not nearly as robust as in the adult literature. For this reason, screening serum lactates in children should not be routine. More important, a serum lactate in the 18–36 mg/dL group (2–4 mmol/L) should not falsely reassure the practitioner that a child is not sick, as there were a number of deaths in this group.
While screening pediatric patients for sepsis with serum lactates is not routine, there are data to suggest that trending lactates for clearance is associated with less persistent organ dysfunction at 48 hours.6
Conclusion: Serum lactate measurements in children do not provide the robust sepsis risk stratification demonstrated in the adult literature. While hyperlactatemia (>4 mmol/L) may suggest a sicker patient, it is very important to recognize that a normal or intermediate lactate level should not falsely reassure you that a child is not sick.
Question 2: Do prophylactic antibiotics decrease the likelihood of drowning-associated pneumonias in children?

ILLUSTRATION: Shutterstock.com
In general, the data are scarce and based on a mixture of adult and pediatric patients. One of the earliest studies on this topic was a retrospective study of 91 consecutive children and adults (ages 1 to 79).7 Of these patients, 81 of 91 (89 percent) survived, and they appeared to have a variety of presentations, with 33 patients requiring intubation. The data are very limited, and the authors noted, “More patients died who received prophylactic antibiotic therapy [7 of 54 (13.0 percent)] than did those from whom such therapy was withheld until gram staining, culture, and the clinical course suggested the presence of active infection [2 of 36 (5.6 percent)].” There was one patient unaccounted for and no mention of statistical significance. They did not mention the patients’ ages or the severity of illness for patients who received prophylactic antibiotics.
An older retrospective study of 40 patients, with 33 of the patients younger than 17 years, found that prophylactic antibiotics given to 31 of 40 patients “had no apparent benefit” in the patient population.8 An additional retrospective study of 125 submersion victims included an unspecified breakdown of children versus adults and found no significant benefit from prophylactic antibiotics.9
Conclusion: While there has been no reported benefit from prophylactic antibiotics in cases of near drowning, there have been no prospective trials assessing this topic. Current expert consensus on this very limited topic by the Wilderness Medical Society recommends that “there is no evidence to support empiric antibiotic therapy in the treatment of drowning patients.”10 Thus, the use of prophylactic antibiotics remains at the discretion of the treating physician.
 Dr. Jones is assistant professor of pediatric emergency medicine at the University of Kentucky in Lexington.
Dr. Jones is assistant professor of pediatric emergency medicine at the University of Kentucky in Lexington.
 Dr. Cantor is professor of emergency medicine and pediatrics, director of the pediatric emergency department, and medical director of the Central New York Poison Control Center at Upstate Medical University in Syracuse, New York.
Dr. Cantor is professor of emergency medicine and pediatrics, director of the pediatric emergency department, and medical director of the Central New York Poison Control Center at Upstate Medical University in Syracuse, New York.
References
- Shapiro NI, Howell M, Talmor D. A blueprint for a sepsis protocol. Acad Emerg Med. 2005;12(4):352-359.
- Dugas MA, Proulx F, de Jaeger A, et al. Markers of tissue hypoperfusion in pediatric septic shock. Intensive Care Med. 2000;26(1):75-83.
- Reed L, Carroll J, Cummings A, et al. Serum lactate as a screening tool and predictor of outcome in pediatric patients presenting to the emergency department with suspected infection. Pediatr Emerg Care. 2013;29(7):787-791.
- Scott HF, Donoghue AJ, Gaieski DF, et al. The utility of early lactate testing in undifferentiated pediatric systemic inflammatory response syndrome. Acad Emerg Med. 2012;19(11):1276-1280.
- Scott HF, Brou L, Deakyne SJ, et al. Association between early lactate levels and 30-day mortality in clinically suspected sepsis in children. JAMA Pediatr. 2017;171(3):249-255.
- Scott HF, Brou L, Deakyne SJ, et al. Lactate clearance and normalization and prolonged organ dysfunction in pediatric sepsis. J Pediatr. 2016;170:149-155.e1-4.
- Modell JH, Graves SA, Ketover A. Clinical course of 91 consecutive near-drowning victims. Chest. 1976;70(2):231-238.
- Oakes DD, Sherck JP, Maloney JR, et al. Prognosis and management of victims of near-drowning. J Trauma. 1982;22(7):544-549.
- van Berkel M, Bierens JJ, Lie RL, et al. Pulmonary oedema, pneumonia and mortality in submersion victims; a retrospective study in 125 patients. Intensive Care Med. 1996;22(2):101-107.
- Schmidt AC, Sempsrott JR, Hawkins SC, et al. Wilderness Medical Society practice guidelines for the prevention and treatment of drowning. Wilderness Environ Med. 2016;27(2):236-251.
Pages: 1 2 3 | Multi-Page



No Responses to “Sepsis Screening Tools for Pediatric Patients and Prophylactic Antibiotics for Near Drowning Questioned”