The Targeted Temperature Management (TTM) trial published in the New England Journal of Medicine in November 2013 was perhaps the most important article of the year in resuscitative and critical care medicine.1
Explore This Issue
ACEP Now: Vol 33 – No 10 – October 2014In the setting of advanced post-arrest care and a protocolized neuroprognostication system, this large, multinational randomized controlled trial compared two targeted temperature management strategies (33°C versus 36°C) in out-of-hospital post-arrest patients and found no significant difference in mortality between the two groups.
If you haven’t heard about this study yet, this is not an introductory piece. But that’s okay. The website www.EMCrit.org offers an enormous set of resources about this trial and others dealing with therapeutic hypothermia (TH) that came before it. The purpose of this piece, rather, is to discuss some important details of the study and attempt to answer the question, “So, what do we do now?”
Basis for Mild Therapeutic Hypothermia and TTM Trial
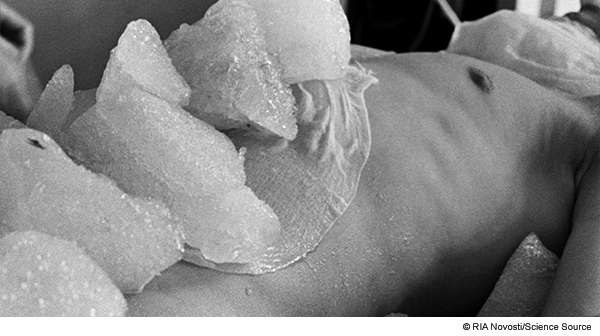
TH in post-arrest patients has been used for decades; it’s a practice largely based on theory, animal models, and retrospective analyses.2 In 2002, two groundbreaking randomized control trials, Bernard and Hypothermia After Cardiac Arrest (HACA), demonstrated a benefit in the number of patients discharged neurologically intact when cooling patients with initial shockable ventricular dysrhythmias. These patients were cooled to mild hypothermic temperatures of 32–35°C for 12 and 24 hours after arrest versus then-standard-of-care ad-lib temperatures. The control groups did not receive active temperature control.3,4
Further nonrandomized studies have shown similar survival benefit in terms of relative risk in other arrest rhythms and groups, making moderate hypothermia the standard of care for out-of-hospital post-arrest patients around the world.5
36°C may be as good as 33°C with potentially fewer complications…it’s still mild hypothermia, it’s still preventing fever.
A 2011 Cochrane review estimates that for every six patients treated with mild hypothermia after cardiac arrest, one receives survival benefit, making TH one of the most effective interventions in our modern post-arrest care arsenal.6
However, moderate TH does not come without potential adverse events such as sepsis, coagulopathy, electrolyte imbalance, and life-threatening dysrhythmia, to name a few.7
That’s why this trial is such a big deal. The TTM trial suggests that by actively preventing fever with mild hypothermia at 36°C, we can achieve the same mortality benefit without added adverse consequences.
Online Reaction & Reception
Almost immediately after its publication, the TTM trial gained widespread attention in the FOAMed and social media communities, igniting discussion and debate with both praise and caution for its future implication on clinical practice.
Pages: 1 2 3 4 | Single Page




One Response to “Research on Therapeutic Hypothermia for Post-Arrest Patients Helps Refine Temperature-Management Strategies”
October 26, 2014
ekulstadFunny that despite the beautifully articulated analysis, even the headline in the ACEP eNow mailing sorta gets it wrong: “ADVANCES IN ED CRITICAL CARE – Chill on Therapeutic Hypothermia?”