The Case
A previously healthy, fully immunized five-year-old boy presents to the pediatric emergency department with three days of fever and a progressive rash. Symptoms started with fevers to 104°F, a few “flat red spots” on his cheeks and behind his right ear, and bilateral injected eyes. The next day, he was seen by his primary doctor, who prescribed ofloxacin eyedrops for a presumed infection. That night, he developed crusting at his lips, redness and swelling of his palms and soles, and red patches on his trunk. On the morning of presentation, he had a few episodes of nonbloody, nonbilious emesis and complained of pain with urination and pain with swallowing. He was refusing to open his eyes to receive the prescribed medication.
Upon presentation to the ED, his blood pressure is 116/76, his pulse is 148, his temperature is 104.4°F, his respiratory rate is 21, and his SpO2 is 97 percent.
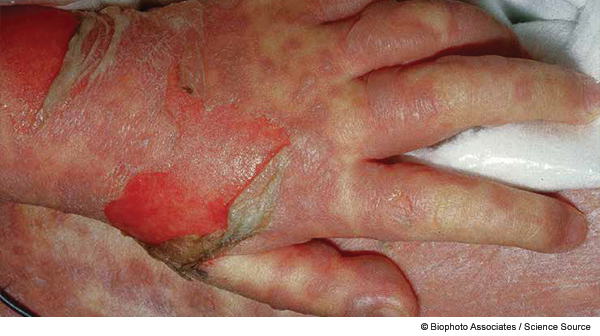
He is an alert, tearful boy, persistently keeping his eyes closed and clearly uncomfortable. There is left anterior cervical lymphadenopathy without a single large node and full range of motion at the neck. On ocular exam, the patient squeezes his eyelids shut and cries. Mildly edematous eyelids are pried open, and there is scant white/yellow discharge bilaterally. The pupils are equal and reactive to light, with bright red injection of the conjunctiva bilaterally. The lips are cracked and erythematous. There is a strawberry tongue and some desquamation at the buccal surfaces. There is tachycardia but no murmurs, rubs, or gallop with a brisk capillary refill. No respiratory distress is present. Abdominal and genitourinary exams are unremarkable for this circumcised male. There is mild bilateral hand swelling. There is an erythematous macular rash at the bilateral cheeks, chest, and back, as well as palmar erythema.
While in the ED, the patient is given a 40 cc/kg normal saline bolus, morphine, and acetaminophen, which make him more comfortable. He is started on maintenance IV fluids and ceftriaxone empirically. Vital signs normalize.
Background and Pathophysiology
Toxic epidermal necrolysis (TEN) is an infrequent medical emergency (0.4–1.3 cases per million per year worldwide) with high mortality.1 It is characterized by fever and widespread tender involvement of the epidermis and mucous membranes resulting in exfoliation. Stevens-Johnson syndrome (SJS) is categorized as less than 10 percent skin involvement, while TEN involves more than 30 percent of the body surface area. Both diseases are seen as a spectrum of a single process.2 Mortality is often due to systemic infection or multisystem organ failure.
All skin and mucous membranes are susceptible to involvement. Mucous membrane involvement often precedes skin lesions, appearing with the prodromal illness (eg, fever, cough, sore throat). The rash often begins as a poorly defined erythematous macular rash that progresses in hours to days. This patient has TEN “without spots,” which is the less-common form of TEN, lacking target lesions. This is compared to TEN “with spots,” which features widespread erythematous or purpuric macules with blistering on the macule.2
Drugs are most often implicated in TEN. One study at a major pediatric burn intensive care unit cited medication use in all 15 described cases.3 The most common drugs cited are antibacterials, sulfonamides, nonsteroidal anti-inflammatory drugs, allopurinol, disease-modifying agents, anti-epileptics, anti-retroviral agents, and corticosteroids.4 Infectious causes including mycoplasma and herpes virus have also been documented.
Are there any confirmatory tests for TEN that can be performed in the emergency department?
- The diagnosis of TEN is generally clinical. The patient’s history (particularly medication history) and physical exam (particularly head, eyes, ears, nose, throat, genitourinary, and skin) are imperative.
- The only confirmatory test is histopathologic analysis of a skin biopsy; full thickness epithelial necrosis is diagnostic.
- There is no definitive laboratory or imaging study to make the diagnosis.
- As the disease progresses with multiorgan involvement, more laboratory test abnormalities may be identified.
What clinical clues suggest the diagnosis of TEN in a child?
- Increased salivation and decreased appetite from oral involvement.
- Painful micturition due to urethral involvement.
- Profuse diarrhea due to enteral involvement.
- Respiratory distress due to involvement of the bronchial epithelium.
- Ocular lesions, which may indicate a higher chance for morbidity due to tearing of the epidermis leading to conjunctival erosions, keratitis, and corneal erosions.
What else should be considered when treating patients diagnosed with TEN?
Differential diagnosis should include Kawasaki disease, staphylococcal scalded skin syndrome, toxic shock syndrome, disseminated adenovirus infection, infectious conjunctivitis, Reiter’s syndrome, hypersensitivity vasculitis, erythema multiforme, exfoliative conjunctivitis, disseminated herpes infection, and measles.
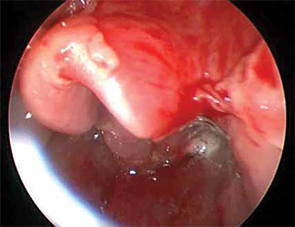
Figure 1: Supraglottic desquamation of lingual surface of epiglottis and vallecula.

Figure 2: The patient’s trachea appears normal.
What immediate threats must be addressed in a patient with TEN?
In the ED, the treatment of the patient with suspected SJS/TEN is akin to that of a patient with severe burns.
- Discontinue any identified offending agent early.
- Consider early transfer to a burn unit because these interventions are associated with improved outcomes.5
- Early fluid resuscitation is imperative in any patient who appears to be in shock.
- Broad-spectrum antibiotic administration is warranted if the child meets criteria for sepsis or if infectious etiology of symptoms is considered likely; however, routine antibiotic administration is not indicated as in the case of severe burns.
- Manage fluids and electrolytes, provide adequate analgesia, prevent secondary infection, and keep the patient warm.
Other than supportive care, what can be done for a patient with TEN?6
Therapeutic measures for TEN remain controversial.
- Most dermatologists at this time do not advocate corticosteroid use.
- Intravenous immunoglobulin (IVIG) is often utilized in treatment protocols, but no randomized controlled trials to date have shown definitive benefit.
Case Resolution
While the patient is on the floor, an echocardiogram is scheduled for the next day to check for potential Kawasaki disease. Infectious disease and dermatology are consulted and scheduled to see the patient the next day. Urology is consulted for placement of a urethral catheter due to lack of urine output and urethral pain. By the eighth hour of hospital admission, the rash has quickly changed quality from macular to bullous and vesicular and has spread to involve the majority of surfaces of his body, including the palms and soles. The patient is transferred to the pediatric ICU with a new oxygen requirement of 0.5 L by nasal cannula and concern for upper airway involvement with TEN.
Shortly after transfer to the pediatric ICU, the patient’s respiratory status worsens. He is taken to the operating room with ENT and anesthesia for elective intubation for airway protection. Upper airway evaluation shows desquamation of the supraglottic structures without tracheal involvement. The patient is diagnosed with TEN secondary to mycoplasma infection based on positive immunoglobulin G and immunoglobulin M titers. The patient receives a three-day course of IVIG empirically. Ophthalmologic evaluation confirms a left corneal abrasion and extensive ocular involvement, also consistent with TEN. Four days into the hospital stay, the patient has a cardiac arrest. The suspected culprit is a mucous plug in the endotracheal tube. He subsequently has bilateral chest tubes placed for pneumothoraces. Throughout his hospital stay, he has several episodes of fever and is on acyclovir, azithromycin, vancomycin, and cefotaxime at varying points.
The patient is discharged after a four-week hospital stay to a pediatric rehabilitation facility. Ophthalmologic, dermal, and respiratory findings have all resolved, and the patient is back to playing video games and attending kindergarten, as he did prior to the acute illness.
Dr. Kosoko is a postdoctoral fellow in pediatric emergency medicine and global health at Baylor College of Medicine/Texas Children’s Hospital. She practices adult and pediatric emergency medicine in Houston and can be reached at aakosoko@texaschildrens.org.
Dr. Kaziny is an assistant professor of pediatrics in the section of emergency medicine at Baylor College of Medicine. He practices pediatric emergency medicine at Texas Children’s Hospital.
References
- Abood GJ, Nickoloff BJ, Gamelli RL. Treatment strategies in toxic epidermal necrolysis syndrome: where are we at? J Burn Care Res. 2008;29:269-276.
- Bastuji-Garin S, Rzany B, Stern RS, et al. Clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Arch Dermatol. 1993;129:92-96.
- Spies M, Sanford AP, Aili Low JF, et al. Treatment of extensive toxic epidermal necrolysis in children. Pediatrics. 2001;108:1162-1168.
- Roujeau JC, Kelly JP, Naldi L, et al. Medication use and the risk of Stevens-Johnson syndrome or toxic epidermal necrolysis. N Engl J Med. 1995;333:1600-1607.
- Endorf FW, Cancio LC, Gibran NS. Toxic epidermal necrolysis clinical guidelines. J Burn Care Res. 2008;29:706-712.
- Ferrandiz-Pulido C, Garcia-Patos V. A review of causes of Stevens-Johnson syndrome and toxic epidermal necrolysis in children. Arch Dis Child. 2013;98:998-1003.
Pages: 1 2 3 4 | Multi-Page






No Responses to “Recognize Pediatric Toxic Epidermal Necrolysis Symptoms, Manage Disease”