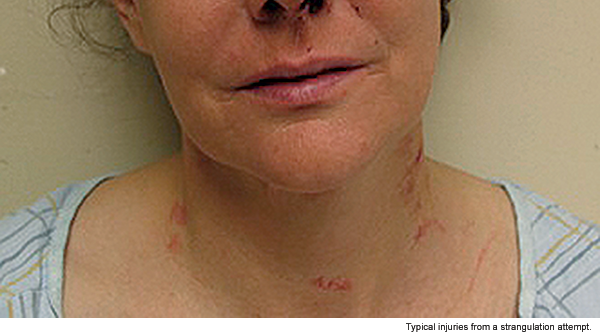
Women are killed by intimate partners more often than by any other type of perpetrator. One in three female homicide victims is killed by her current or former partner. The overwhelming majority of these women are seen in EDs in the year prior to their homicide, making the ED an ideal location for interpersonal violence (IPV) screening and intervention.
Explore This Issue
ACEP Now: Vol 33 – No 05 – May 2014Emergency physicians should maintain a high index of suspicion for IPV and screen all patients, male and female, who may be at risk. Circumstances that should increase concern for IPV include multiple visits for injuries, multiple injuries in various stages of healing, patterned injuries such as slap marks and defensive injuries, injuries inconsistent with the history provided, and an overbearing significant other. When evaluating injuries, the potential for IPV must be top of mind or it’s guaranteed to be missed. Several validated screening tools are available, and EDs should have policies and procedures in place for IPV screening and referral to appropriate local resources. Patients should not be screened in the presence of friends or family members.
If the IPV screen is positive, patients should be screened for risk factors for lethality. Risk factors for domestic violence homicides include attempted strangulation, estrangement from the abuser, and pregnancy. The risk of becoming an attempted/completed femicide (the killing of women) victim is three times higher for women abused during pregnancy and seven times higher for nonfatal strangulation victims. Perpetrator red flags include alcohol/drug abuse, access to firearms, use of firearms during previous domestic violence incidents, and unemployment. Perpetrator problem drinking was associated with an eightfold increase in partner abuse and a twofold increased risk of femicide/attempted femicide.
The emergency physician should thoroughly document injuries, specifically paying attention to location, size, color, and shape. Photographs of injuries can be valuable and should be placed in the medical record per hospital policy. Documentation may be the key to saving a life.
Police reporting requirements regarding IPV vary from state to state, and emergency physicians should know the laws in jurisdictions where they practice.
Resources for More Information
- Campbell JC, Webster D, Koziol-McLain J, et al. Risk factors for femicide in abusive relationships: results from a multisite case control study. Am J Public Health. 2003;93:1089-1097.
- Gazmararian JA, Petersen R, Spitz AM, et al. Violence and reproductive health: current knowledge and future research directions. Matern Child Health J. 2000;4:79-84.
- Glass N, Laughon K, Campbell J, et al. Non-fatal strangulation is an important risk factor for homicide of women. J Emerg Med. 2008;35:329-335.
- McFarlane J, Campbell JC, Sharps P, et al. Abuse during pregnancy and femicide: urgent implications for women’s health. Obstet Gynecol. 2002;100:27-36.
- Sharps PW, Campbell J, Campbell D, et al. The role of alcohol use in intimate partner femicide. Am J Addict. 2001;10:122-135.
- Tjaden P, Thoennes N. Extent, nature, and consequences of intimate partner violence. National Institute of Justice and the Centers for Disease Control and Prevention. 2000, NCJ 181867.
- Zawit MW. Violence between intimates. US Department of Justice, National Institute of Justice and the Centers for Disease Control and Prevention. 1994, NCJ 149259.
 Dr. Riviello is professor of emergency medicine at Drexel Emergency Medicine in Philadelphia. He is board certified in emergency medicine and has a master of science in forensic medicine from Philadelphia College of Osteopathic Medicine.
Dr. Riviello is professor of emergency medicine at Drexel Emergency Medicine in Philadelphia. He is board certified in emergency medicine and has a master of science in forensic medicine from Philadelphia College of Osteopathic Medicine.
Pages: 1 2 | Multi-Page






No Responses to “How to Recognize and Act on Risk Factors for Domestic Violence Homicide”