
As recently as 15 years ago, the approach to pain management was a symptomatic one, whereby the symptom of pain was hidden or minimized with a general analgesic such as an opioid or acetaminophen. Additional pain relief was sought by treating the underlying disease under the assumption that the pain would resolve if you did so.
Explore This Issue
ACEP Now: Vol 34 – No 02 – February 2015The symptomatic approach has been almost completely replaced by a mechanistic approach. With this approach, the neurobiological mechanism creating the pain is identified and neutralized with a targeted medication. Although far more applicable in managing chronic pain, the mechanistic approach was first seen in acute pain settings. Witness the change from opioids to dopamine antagonists (eg, chlorpromazine, prochlorperazine, metoclopramide) and serotonin agonists (eg, triptans, ergotamines) for migraine and other vascular headaches. The role of prostaglandins in smooth muscle tension has resulted in the use of nonsteroidal anti-inflammatory drugs (NSAIDs) for renal and biliary colic as well as for severe menstrual cramps. Anticholinergic agents can be effective for both intestinal cramps (hyoscine) and large muscle spasms (benztropine). The indications for the primary use of an opioid in emergency medicine have been refined; there are many fewer indications than before, making their use even more justifiable in these specific instances (eg, extremity fractures, visceral pain, vaso-occlusive crisis).
Pain in the ED
In chronic noncancer pain, specific neurotransmitters and nerve channels have been relatively well-established. In neuropathic pain, either a sodium channel (tricyclic) or a calcium channel (gabapentanoid) blocker serves as first-line therapy, with opioids relegated to third- or fourth-line treatment. In diffuse widespread pain such as fibromyalgia, opioids are not recommended at all, with NSAIDs, tricyclics, or gabapentanoids being the optimal choices.
The indications for the primary use of an opioid in emergency medicine have been refined; there are many fewer indications than before, making their use even more justifiable in these specific instances (eg, extremity fractures, visceral pain, vaso-occlusive crisis).
In managing trauma patients, the last few years have demonstrated that the addition of low-dose (analgesic dose) ketamine serves to decrease the dosing requirements of opioids to control pain. It also serves to block N-methyl-D-aspartate (NMDA) release, thereby decreasing wind-up (pain after discharge and the risk of development of chronic pain). For procedural analgesia, ketamine and nitrous oxide serve as excellent alternatives to opioids. Ketamine, in an analgesic dose (0.2–0.3 mg/kg), seems to lead to less oxygen desaturation and hypoventilation when combined with a sedative than when an opioid, such as fentanyl, is used. The use of “ketofol,” a combination of ketamine and propofol in the same syringe, seems to offer no added value over giving a single dose of ketamine followed by the titration of an ultrashort-acting sedative such as propofol or methohexital.
Nitrous oxide was widely available in emergency departments 20 to 30 years ago in North America, but it fell out of favor for two reasons: misuse by staff and variable effectiveness in patients. Both of those problems were the result of trying to make use of a 50/50 mixture (nitrous and oxygen). Use of the 70/30 mixture has provided solutions to both problems: the stronger mixture does not lead to euphoria but rather unconsciousness, making it rather evident who might be trying to misuse it! Analgesic effectiveness is almost 100 percent with the 70/30 mixture, and it is widely used in Australia as a result. It is almost omnipresent in Canadian pediatric EDs as well. Current regulations already in place in the United States for other procedural sedation medications should allow a relatively easy process to reintroduce nitrous oxide into emergency departments. Indications for nitrous oxide’s use rapidly come to mind because of its rapid-on, rapid-off effect. They include catheter placement in cognitively impaired children, casting a pain fracture, and disimpaction, to name a few.
In Europe, where experience now exceeds three years, IV acetaminophen is used routinely in acute pain management as part of a multi-medication approach.
The introduction of IV acetaminophen in the past two years has provided yet another option for acute pain management. In studies to date, 1 g IV of acetaminophen appears to have an analgesic impact almost equivalent to 10 mg morphine. Of course, the same was also said of ketorolac when it was introduced to the market. In Europe, where experience now exceeds three years, IV acetaminophen is used routinely in acute pain management as part of a multi-medication approach. Start with acetaminophen except in obvious severe pain (polytrauma, fractures, etc.) and add an opioid if required. Even in patients requiring opioids, acetaminophen is used, if only to minimize initial dosing of all medications, thus minimizing adverse events from any one agent. Evidence about the safety of repetitive doses of IV acetaminophen does not yet exist. Evidence suggests that 2 g by mouth as a one-time dose would probably be just as effective.
The use of regional anesthesia will be discussed in a future article because it, too, can play an important role in pain management of fractures and in procedures.
After Discharge
Concern over opioid misuse is at its highest when discharge prescriptions are written. First consideration should be to avoid prescribing the opioid most misused in your community. Each community chooses its opioid. Within a 60-mile radius of where I have worked, patients have told me that “only idiots” abuse any opioid other than “fill in the blank.” Heroin, oxycodone, meperidine, hydromorphone, fentanyl, dextromethorphan—they all have been abused, but usually only one is abused in any given community. This is primarily due to control of the drug scene by one gang or another. If opioids do have to be prescribed, limit dosing to three to four days maximum because follow-up for persistent pain is essential.
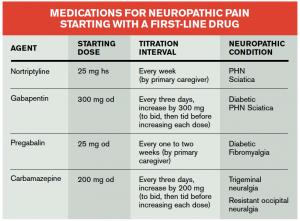
(click for larger image)
Table 1: Abbreviations: hs=at bedtime, od=once per day, bid=twice per day, tid=three times per day
Newer options that have been promoted include tapendtatol and tramadol. The former has turned out to be a very poor analgesic that costs a lot of money, whereas the latter has not gained much favor in the emergency physician community. Neither is at risk for abuse, and tramadol does offer valid analgesia in many patients. It might be of value to provide it in the ED to see how helpful it is prior to writing a prescription for it.
The NSAID with the best analgesia/anti-inflammatory/safety profile still is ibuprofen. It is the recommended analgesic of choice for dental pain. For new onset or a flare of chronic sciatica or other neuropathic pain, short-acting opioids will rarely help the patient. A combination of a NSAID with a tricyclic (nortriptyline is less sedating) is probably best. It is important to note that the starting dose of the tricyclic should be 25 mg at bedtime, rapidly titrated over seven to 10 days to at least 75 mg and with follow-up with a primary care provider. Carbamazepine for tic douloureux should be started at 200 mg and titrated up 200 mg every three days to effect, again with follow-up within one week. Initiation of either a tricyclic or a gabapentanoid (gabapentin 300 mg, increasing by 300 mg every three days to effect, or pregabalin 25 mg a day with much slower ramp up due to side effects) for postherpetic neuralgia (PHN) is an excellent option. See Table 1 for more recommendations for treating neuropathic pain.
Summary
Many nonopioid options exist, but to use these medications optimally and safely, a much greater understanding of pain mechanisms is required. Opioids have their place but a much smaller one than what was seen in the nondiscriminate symptomatic approach era.
 Dr. Ducharme is editor in chief of the Canadian Journal of Emergency Medicine and clinical professor of medicine at McMaster University in Hamilton, Ontario.
Dr. Ducharme is editor in chief of the Canadian Journal of Emergency Medicine and clinical professor of medicine at McMaster University in Hamilton, Ontario.





15 Responses to “Non-Opioid Pain Medications to Consider for Emergency Department Patients”
February 16, 2015
ALgreat overview, thanks. I do have concerns about tramadol because it is a drug of abuse and risky for serotonergic complications//interactions.
February 17, 2015
Jim DucharmeI understand your concern re misuse of tramadol, and its low threshold of toxicity if taken as an overdose – its seizures are hard to control.
Comparatively to hydromorphone and oxycodone the % of people becoming addicted to a Rx opioid is still lower with tramadol (about 1/4 the rate). It is at best a moderate analgesic so is a 2nd or 3rd line choice. I have had others echo your concern about misuse – in retrospect I should have worded that sentence better
February 24, 2015
chris robchristine robinhi,
I work in Qc province. here tramadol isn’t covered.
we dont have acces to Iv tylenol in our hospital. altough thinking about introducing it..
is 2g of tylenol po really as effective? is it safe?
are the evidence convincing?
thank you
February 25, 2015
Ryan RadeckiHi Jim – splendid overview, appreciate the fantastic work you do on these important topics.
Would just like to point out, for intravenous acetaminophen (Ofirmev), there are substantial charges to the patient associated with its use in the U.S., and, even when charges aren’t part of the equation, it’s still substantially more expensive than other intravenous or oral alternatives. Until it is available in the distant future as a less-costly generic, do you still feel as though it offers substantial advantages over oral acetaminophen preparations – or some of the alternative agents – warranting its use?
This question also comes up due to a current ketorolac shortage, for which Ofirmev has been suggested as an alternative.
March 2, 2015
Larry A. Bedard, MD FACEPOverall an excellent article, although I was surprised Dr. Ducharme didn’t mention medicinal marijuana. Medicinal marijuana is now legal in 23 states and the District of Columbia. A June 2014 article in JAMA concluded: ” States with medical cannabis laws had a 24.8% lower mean annual opioid overdose mortality rate compared with states without medical cannabis laws. Medical cannabis laws are associated with significantly lower state-level opioid overdose mortality rates.” A 2009 study at the University of California San Diego for HIV patients with neuropathic pain found a 30% reduction in pain with the use of cannabis. Mood and daily functioning improved to a similar extent. The study concluded:” Smoked cannabis was generally well tolerated and effective when added to concomitant analgesic therapy in patients with medically refractory pain due to HIV DSPN.” In an May 2013 article in the AMA journal of Ethics reviewing the use of cannabis in neuropathic pain stated: “Overall, the efficacy of cannabis was comparable to that of traditional agents, somewhat less than that of the tricyclics, but better than SSRIs and anticonvulsants, and comparable to gabapentin.”
The October 2010 issue of the CMAJ published research from McGill University entitled “Smoked cannabis for chronic neuropathic pain”, which concluded: “A single inhalation of 25 mg of 9.4% tetrahydrocannabinol herbal cannabis three times daily for five days reduced the intensity of pain, improved sleep and was well tolerated.”
Sativex, the THC-CBD combination in a sublingual spray, is available in Canada to treat cancer pain and neuropathic pain in multiple sclerosis. I wonder if Dr. Ducharme considers this an appropiate drug in the armamentarium of Emergency Physicians.
There is a growing body of medical evidence which supports emergency physicians recommending medicinal marijuana for patients with pain.
Lary A. Bedard, MD
March 4, 2015
Jim DucharmeSome great comments, so let me address them as much as I can:
1) medical marijuana or cannabinoids: this topic makes me nervous. Marijuana is a recognized gateway drug – users have a 140 times greater risk of progressing to ‘harder’ drugs than do those who do not use marijuana. Comparatively, those who drink alcohol have only a 10 times greater risk. Synthetic cannabinoids do have a place in chronic pain, but as a 3rd or 4th line option. Due to a very high rate of sedation, titration to analgesic effect usually takes 6-8 weeks – so they are not valid choices for acute pain. Marijuana when smoked is almost impossible to titrate to get analgesic effect without also getting psychotropic effects – which honestly is why almost everyone wants the ‘medication’ in the first place. So while I recognize its role in chronic pain and in chemotherapy, I do not support any role for acute pain at this time.
2) 2 g of PO acetaminophen: a one time dose is certainly safe. The question – as brought to my attention by a toxicologist (and a good friend) – is what message will we be giving the patient? We are limiting total daily dose to 4 g…..if a patient sees we are giving 2 g PO, will there not be the risk that the average patient does so every 4 hours when at home? A great concern, for which I have no possible reply at this point in time.
3) Cost of IV acetaminophen should not be an issue; it should only be used when PO is not allowed or when concerned about adverse effects of other analgesic options. IV acetaminophen if combined with another analgesic will certainly allow lower doing of that analgesic and thus decrease AE’s. It should not become ago to first line drug in all settings. Parenteral NSAIDs have almost no benefit over oral ones – comparing 600 mg ibuprofen PO to 30 mg ketorolac IV in renal colic: ketorolac offer pain relief about 20 minutes faster but has an effect that is about the same as oral ibuprofen, while lasting for a shorter period of time that oral ibuprofen.
Thanks again for the great comments and insights!
March 13, 2015
Joshua Russell, MDHi Jim,
Great column!
I was hoping you could help direct me to a ketamine as analgesia protocol used in your hospital system or another one that you’re familiar with. I’m an ER doc in Washington state and on P&T committee and am fighting about/collegially debating over the safety of ketamine for analgesia at low doses (0.15-0.3 mg/kg) with the anesthesiologist chair of the committee.
As it stands, ketamine use here of any kind is defined as a sedation, when it is clearly non dissociative at such doses and I’d imagine much less likely to cause airway compromise, apnea etc.
Any protocols/resources that I could use as ammunition to liberalize our policy on such a safe and effective analgesic would be very, very helpfu!. Thanks for your help and keep up the good and important work!
Josh R.
Vancouver, WA
March 15, 2015
Rob OelhafDr. Ducharme, I have been following your essays on this topic for a while, and this one is the most balanced and on point thus far. I am very grateful for your boldness and persistence in discussing this.
I wholeheartedly support your anxiety regarding marijuana. I echo your statement, and add that one should not smoke one’s medicine (I concede there is movement toward aerosolization, but there must be associated costs). Additionally, where are the dronabinol advocates in this sea of banner-waving marijuana smokers? Dronabinol has been Schedule III in the US since the late 1980s. Some have suggested the effect is more durable and more intense than smoked leaf. I have to believe our lack of dronabinol advocacy has allowed the marijuana legalization movement to gain traction.
I also need to comment on the community focus on a certain opioid. This may be genetic response/effectiveness. A study of South African prescribing patterns found that outpatient prescriptions for opioids very frequently contained codeine and meprobamate, medications that I was trained to never bother prescribing because other opioids were safer and more effective. I grant that this is a 1995 study, but the difference between South African and US prescribing is striking. Which begs the question, why are US doctors, time and again, so relatively ineffective at treating African American pain? Can it be that we are trained to not prescribe the agents that actually work in this population?
I Truter and TJ Kotze, 1995. Prescribing of analgesic agents in a South African patient population. Annals of Pharmacotherapy 29:1302-1303
March 18, 2015
henry richterThis is yet another article designed to convince young doctors- as if they were not already convinced- that appropriate symtomatic pain relief can be deferred for days, months, or forever. Reading this magazine, the other free EM magazines that show up in my mail box monthly, or the ACEP journal, all I see are excuses not to treat pain. In over thirty years as an EM physician who faithfully reads the EM literature, I can NEVER recall seeing an article about the ED presentation of psuedoaddiction. Is not the bias self-evident, Dr. Ducharme? My personal experience is that psuedoaddiction is present in the majority of patients seeking pain relief in the ED. It takes an extra 2 or 5 minutes with the patient to figure this out. Tough, sorry, that’s your job.
Instead, I see self justifying excuses not to give narcotics. It makes the doctor feel better, like he/she is helping mankind, but ignores the patient in front of him.
Don’t get me wrong. I have been giving 1 gram of Tylenol and 600 mg of Motrin po to all my ED patients who are not vomiting as soon as I see them in the ED. I have been doing this for years. I think this regimen has reduced narcotic usage in patients with abdominal pain or orthopedic pain, and to some degree has served as a teaching mechanism for patients to self treat themselves at home. There are medications for acute treatment of migraines that work better than narcotics, etc.
The table on page 7 is fascinating for what it leaves out. Most important, the high doses of Tegretol or Pamelor required to address pain have simply intolerable side effects. Second, when have you ever seen a patient in the ED on substantial doses of gabapentin or pregabalin. The majority are on the lowest doses possible, and these patients continue to suffer. In fact, I would say that individualized titration of all four medications in the table is simply not done by any doctor involved: the PCP, specialist or ED doctor. I challenge anybody reading this comment to take 150 mg of Pamelor daily; let’s see if you can tolerate what you pontificate.
The scripts are pompous exercises in excuses not to delve into the patient deeply enough to understand the drug seeking. They are self justifications to allow suffering. Be careful what you ask for, doctors: someday you will show up in the ED with your own kidney stone. I suspect you will grovel for the close to immediate relief that Fentanyl or Diluadid offer.
Dr. Ducharme, perhaps your next article should be on psuedoaddiction. I eagerly await it.
November 2, 2017
Kathleen D WilhoitThank you! My best friend is dead because the doctor was more worried about her maybe getting addicted than treating her pain. A combination of 7 herniated discs, and diabetic nerve pain so bad she couldn’t walk, but a prescription for trammadol was all that was offered. Tylenol? Really? Instant karma is what I pray for, for this current mass hysteria over treating patients with stronger meds.
March 19, 2015
Jim DucharmeI would like to address comments from Dr Richter where he feels there are “self justifying excuses to not use narcotics” in EDs and in my text. Let me be clear on a few points:
1) many patients come in with what appears to be drug seeking behavior. The large majority of those are people acting out because the health care community has failed to address their pain with normal behavior. This is pseudoaddiction. We have to be good enough to distinguish these people suffering from those who wish to misuse drugs – that is on us.
2) although there has been an (appropriate) increase in our arsenal of possible analgesics, opioids are still the preferred medication for acute severe pain when a specific medication targeting a specific pain pathway will not work.That I personally use less opioids in my practice compared to 10 years ago in no way means my patients’ pain is not well addressed.
3) part of oligoanalgesia is under dosing – we have been guilty of this with opioids for decades, so it is not surprising that many physicians provide inadequate doses of non-opioid analgesics
4) getting to the proper dose however is a slow process. You do not get someone to 175 mg nortryptilline per day in a week; that is equally true for getting someone up to 3 gms per day of gabapentin. In pain clinics, it may take 2-3 months to get to the right dose while minimizing adverse effects (“start low and go slow”). Such titration is NOT possible for an ED patient – we can only initiate such a medication and arrange for close follow up. Similarly analgesic dosing of ketamine hits a ceiling at about 0.3 mg/kg for after that adverse effects become too severe and frequent. Even with the normal dose range the first dose should be infused over 10 minutes to minimize AEs.
I wish to reiterate therefore that providing analgesic options (including nerve blocks) is so that we can optimize pain relief while minimizing adverse events (including drug diversion and misuse) NOT to justify not giving opioids or to not treat pain.
March 25, 2015
Steve SpontakA bit off topic, but I’m wondering if you could provide a reference to your figures that say that Marijuana users are 140X more likely than non-marijuana users to go on to harder drug use, while drinkers are 10X more likely than nondrinkers (I think this is what you referred to) to go onto harder drug usage. This is something I have always strongly suspected, and continuously had to argue (without stats to back me up) about with my “legalized marijuana” friends and colleagues. I would be interested in seeing the study that came to the stated statistics.
Thanks!
April 12, 2015
Larry A. Bedard, MD FACEPI also would like to see Dr. Ducharme’s reference that marijuana is a gate way drug to harder drug use. The 1972 Schafer Commission in the US, the 1972 La Dain Commission in Canada and the Bain Commission in the Netherlands all debunked the “Marijuana is a gateway drug” theory. All three commissions recommended that decriminalization and legalization. The gateway theory is simply propaganda from Richard’ Nixon’s'”War on Drugs” and Nancy Reagan’s “Just say No!. There is growing evidence the cannabis is an “exit drug.” States that have legalized medicinal cannabis have seen a 25% reduction in opiate OD deaths. In the 1980s when marijuana use significantly declined, cocaine use significantly increased!
Illegal drugs are the gateway to other illegal drugs. Your corner drug dealer doesn’t ask for ID and usually has a variety of other illegal drugs. As one patient told me he began using Ecstasy when his marijuana connection gave him some Ecstasy for his 18 birthday. He scored a “home run” with his girlfriend. When he asked for another Ecstasy the cost was $20.00. Drug dealing 101: “The first one’s free, the second one cost you!”
I think Dr. Ducharme is confusing correlation with causation. The most common illegal drug first used is underage drinking of alcohol or smoking of cigarettes. There is a correlation of illegal use of alcohol or tobacco and hard drugs but nobody argues causation.
Larry A Bedard, MD
Excellent article by Dr. Ducharme other than unsubstantiated claim that cannabis makes you 140 times more likely to abuse hard drugs.
May 16, 2015
Andrew CogginsWas inspired. Reflections here:
http://emergencypedia.com/2015/05/14/we-suck-6-tips-for-controlling-pain-in-the-emergency-department/
Thanks for continuing to advocate on this issue!
Andrew
July 24, 2020
Linda KwiatkowskiFrom my experience as a surgeon and a patient with a painful neurologic autoimmune disease, I’ll say that most ER physicians are not educated or up to date on the mechanisms and reality of autoimmune neurologic complications such as sensory ganglionopathy,multiple mononeuropathy, chronic inflammatory demyelinating polyneuropathy, distal axonal sensory polyneuropathy, and peripheral neuropathy, and the sudden onset severe pain patients with Sjogren’s, MS, and Lupus can develop. I had mononeuritis multiplex and the ER physician refused to examine me and laughed as he just sent me out the door. I had to go somewhere else to be treated because if this isn’t treated, one can end up with permanent motor function impairment. There has traditionally been a negative stigma associated with these diseases, and when these patients come in with severe, sudden onset pain, they are treated as drug-seekers and are not given pain relief, or any treatment for the underlying disease. They are told the ER is only for heart attacks and strokes. The pain they experience can be worse and more prolonged than a kidney stone, cancer pain,or post-operative pain, and now we pretend that treating this pain is not important and label these patients permanently in the medical record, which goes on to affect their future care. Throughout the literature, opioids are recommended as part of the treatment for these patients, yet now we refuse to use them. A patient with a progressing, degenerating autoimmune disease that is causing constant deterioration of the nervous system, is suffering and being tortured by the disease, and the last thing to worry about in the immediate crisis period is if that person is going to get addicted to opioids. Some of these patients could really qualify as hospice patients the disease is that bad, and yet we still hold out on the tried and true medications that will ease their suffering. These people are probably the least likely to abuse opioids. This current trend to ignore pain and pretend it doesn’t exist, and to make all patiens with pain into criminals because they could get addicted to pain medicine is such a demonstration of mass hysteria to the point of loss or all common sense and empathy that one day we will look back at this dark period with shame. It’s fine to try to find better non-narcotic opeions for pain control, but for God’s sake, when there is a person with a horrible disease suffering in pain, we have always been there to at least be able to treat that pain even if we haven’t had a cure for that disease. Spend less time reading about IV Tylenol and read about the reality of autoimmune neurologic complications and the pain that these diseases produce that is worse than a kidney stone, surgical pain or pain from cancer. Consider that at least in cancer a patient usually has some option for treatment and may go into remission or be cured, and if not, there is a limited time to the suffering because the patient will likely die from disease in a fairly well-understood period if treatment is not successful. With these AI diseases, patients go on and on slowly deteriorating being treated badly due the the stigma associated with these diseases and the growing hatred towards anyone who has pain and wants to get relief. Why don’t we get rid of all of the alcohol because there are many alcoholics and people dying of alcohol related medical problems? Oh, that has been tried in the past and we know historically how that turned out. You always think it will never happen to you, but any one of these providers who have been brainwashed into ignoring pain and using all sorts of often more dangerous methods to attempt to appear to be doing something, any one of you could end up on the opposite side tomorrow. You will understand things differently once you are the patient and you are the one in pain. Also, we need to stop ignoring the gender bias in treatment. Studies show men get better and faster pain treatment than women. There is that stigma that women are weaker and can’t handle stress and pain and are less believable.
In all my years treating patients, the women were the tough ones, so I don’t understand why this behavior persists. Thank you to the few rational folks who have weighed in. I no longer feel the sense of pride I used to to be associated with the medical profession. I feel I have to apologize for them during this time because we are not doing a good job. And by the way, Medical marijuana has nothing to do with being a gateway drug. When people debate that issue, they are generally talking about recreational, illicit drug use. Here again is ignorance about the true definitions of the somewhat subtle differences between people with real medical problems using medication as presribed to treat a real medical problem and illicit drug use. I agree with the person who makes a good point about what you want to call the gateway for anything. Maybe it’s overeating, smoking, or drinking too much when you go out. What do you want to do, control everyone to the point of some utopian society? It’s never going to happen and that’s a socioeconomic and cultural issue much more than and issue of what our job as doctors is.
Our job as doctors is to treat disease, pain, and suffering. Not to correct all of the socioeconomic and cultural problems that exist. People who take opioids (or marijuana) as directed to treat a medial problem without abusing it, and who function as capable adults do exist. In fact they are the majority. It is arrogant to look at all patients as though they are mentally inferior and have such a lack of self control that they can’t take medication as prescribed without problems. I’m sure you think you’re capable of taking medication as prescribed, and I believe that if any of these “anti-pain treatment” providers were hooked up to something that simulated the pain of many of their patients, they wouldn’t last long before behaving the same way and begging for something to get the pain to stop. That is why torture has always been so effective. Everyone has a breaking point where they just can’t take anymore pain. Pain is torture. If you refuse to really treat it, you are doing harm and you are allowing the torture to persist. The patient never fully recovers from this. There is always damage. People become traumatized after torture. If we always felt it was important to treat before, it is kind of like the psychology of blame to say the problem is that the patients are all so weak and become addicts, when really we need to admit that we probaly weren’t monitoring closely enough when people were having problems and there was really no good system in place to deal with those people, but there have historically always been addicts, and not treating pain in people with real pain is never going to impact that. It’s probably going to create a larger population of angry, traumatized people with nothing to lose. So consider that in the daily “denial of pain” world we are in.