The warm, swollen knee is a common complaint in the emergency department, with joint aspiration being the diagnostic test of choice when a septic arthritis is suspected. Point-of-care ultrasound can accurately determine the presence of a joint effusion as well as guide synovial fluid aspiration.1 The suprapatellar bursa, the largest communicating bursa of the knee joint, allows for a location that is easily visualized with ultrasound and can be rapidly and safely accessed for joint arthrocentesis. A simplified sonographic method for evaluation and aspiration of the knee joint is an important addition for even the most experienced emergency physician.
Explore This Issue
ACEP Now: Vol 34 – No 08 – August 2015Background
The provider must first confirm the presence of an effusion before performing a diagnostic arthrocentesis. Classically, the physical exam findings for a knee effusion are swelling, a decreased range of motion, and a ballotable, or floating, patella. Mimics such as cellulitis, prepatellar bursitis, or abscess that may be difficult to distinguish from joint effusion on physical examination are easily identified with bedside ultrasound.2 Once the presence of a knee effusion has been confirmed, the standard practice for needle arthrocentesis has been a landmark-based approach. Ultrasound has been shown to be effective in identification of knee effusion as well as allow for real-time visualized technique for joint aspiration.3 In the emergency department setting, ultrasound-guided knee arthrocentesis has been shown to help minimize attempts as well as improve procedural confidence in the hands of novice providers.4 Additionally, the suprapatellar approach under ultrasound guidance avoids any tendons or bony or ligamentous structures and facilitates simple and accurate arthrocentesis for the provider.
Mimics such as cellulitis, prepatellar bursitis, or abscess that may be difficult to distinguish from joint effusion on physical examination ar easily identified with bedside ultrasound.
Procedure
Ultrasound Identification of Knee Effusion
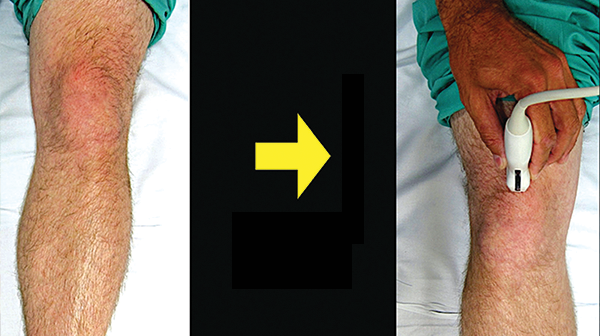
We recommend using the linear transducer (10–5 MHz) for both the identification of the effusion and needle guidance for the arthrocentesis. The patient should be placed in the supine position, with the affected knee slightly flexed (we recommend a small pillow or roll of sheets be placed under the affected knee). Place the linear transducer in the prepatellar fossa in a longitudinal direction with the probe marker caudal (see Figure 1). Identify the patella sonograhically, then slowly slide the probe cephalad until the patella, femur, quadriceps femoris tendon, and fat pad are visualized (see Figure 2). The effusion will appear as an anechoic fluid collection below the fat pad. A small skin wheal of local anesthetic (1–2% lidocaine) injected through a tuberculin syringe should be placed just lateral to the ultrasound transducer (the projected entry point for joint arthrocentesis). We recommend an ultrasound examination of the nonaffected suprapatellar space for comparison.
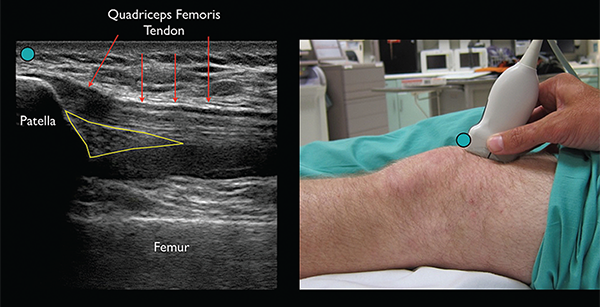
(Click for larger image)
Figure 2. Identify the patella and then slide the transducer cephalad until the approach ultrasound landmarks, including the patella, femur, quadriceps femoris tendon, and fat pad, are appreciated. The effusion will appear as an anechoic (black) space underneath the fat pad. (Green circle indicates ultrasound transducer directional marker.) Credit: Arun Nagdev
Ultrasound-Guided Knee Arthrocentesis
Materials:
- Sterile ultrasound sheath and gel
- 18g 1.5 needle attached to a 5–10 mL syringe
- Chlorhexidine
- Sterile drape
- Sterile gloves
- 30 g tuberculin syringe filled with 1–2% lidocaine or ethyl chloride spray
*Pictures are for educational purposes, and sterile precautions (sterile probe cover, gloves, drapes, etc.) should be used for all joint aspirations.
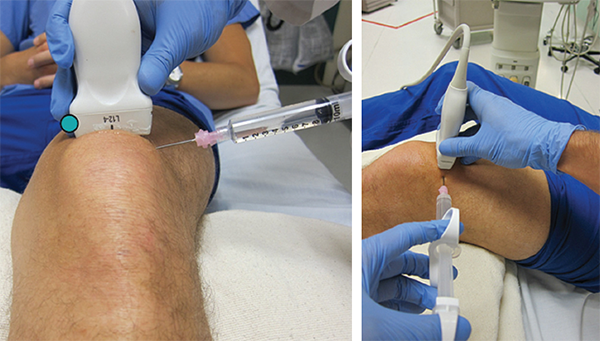
(Click for larger image)
Figure 3. Rotate the probe marker to the patient’s right in order to visualize a transverse view of the prepatellar space with the effusion. Credit: Arun Nagdev
Joint aspiration:
For ultrasound-guided arthrocentesis, we recommend a lateral to medial in-plane technique. With the linear probe in the prepatellar fossa, rotate the probe marker (clockwise) to the patient’s right to obtain a transverse view of the prepatellar space (see Figure 3). A large area around the suprapatellar space should be cleaned and draped in a sterile manner. The ultrasound transducer should be placed in a sterile sheath and then on the sterile field. The ultrasound system should be positioned opposite to the provider so the screen is in the direct line of sight. Using a 10 mL syringe attached to a standard 18g needle, enter the skin in plane and just lateral to the probe at a shallow angle (see Figure 4). The needle will traverse between the iliotibial band (superiorly) and vastus lateralis (inferiorly) without risk for vascular puncture. Clear needle visualization can be achieved by slowly advancing just under the transducer. Gentle aspiration of synovial fluid with needle tip being visualized within the fluid collection will confirm violation of the joint space.
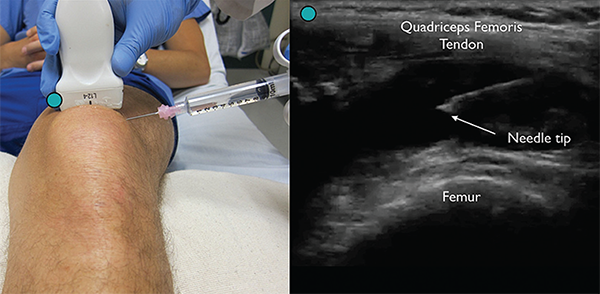
(Click for larger image)
Figure 4. Enter the skin lateral to the probe using an 18g needle attached to a syringe for an in-plane arthrocentesis while visualizing the needle tip. Credit: Arun Nagdev
Summary
Point-of-care ultrasound can be a useful adjunct in the evaluation of the patient with a swollen, painful knee. Ultrasound can identify a suspected knee effusion as well as assist with arthrocentesis. A simplified in-plane technique can easily be incorporated into the evaluation of the patient with a suspected septic knee.
Dr. Johnson and Dr. Lovallo are in the department of emergency medicine at Alameda Health System’s Highland Hospital in Oakland, California.
Dr. Mantuani is an attending physician in the department of emergency medicine and director of internal medicine point-of-care ultrasound at Highland Hospital.
Dr. Nagdev is director of emergency ultrasound at Highland Hospital in Oakland, California, and assistant clinical professor (volunteer) of emergency medicine at the University of California, San Francisco.
References
- Berkoff DJ, Miller LE, Block JE. Clinical utility of ultrasound guidance for intra-articular knee injections: a review. Clin Interv Aging. 2012;7:89-95.
- Adhikari S, Blaivas M. Utility of bedside sonography to distinguish soft tissue abnormalities from joint effusions in the emergency department. J Ultrasound Med. 2010;29:519-526.
- Sibbitt WL Jr, Kettwich LG, Band PA, et al. Does ultrasound guidance improve the outcomes of arthrocentesis and corticosteroid injection of the knee? Scand J Rheumatol. 2012;41:66-72.
- Wiler JL, Costantino TG, Filippone L, et al. Comparison of ultrasound-guided and standard landmark techniques for knee arthrocentesis. J Emerg Med. 2010;39:76-82.
Pages: 1 2 3 | Multi-Page




One Response to “How to Perform Ultrasound-Guided Knee Arthrocentesis”
September 30, 2018
CassandraIs ultrasound injection good for ten knee after a keyhole surgery? I had this surgery for sometimes ago and now my left is severe with pain and decided to go for the ultrasound injection.. I had this injection on my shoulder and is good. I had it twice and never back again.So thinking of having one on my knee. Can you
Advise please thanks.