The Case
A 26-year-old female presents to the emergency department, stating that her husband assaulted her. She complains of headache and sore throat. When directly questioned, she states, “He choked me so bad, I thought I was going to die. I might have blacked out for a minute. It really hurts to swallow.”
Explore This Issue
ACEP Now: Vol 38 – No 04 – April 2019Strangulation is a form of asphyxia, characterized by closure of the blood vessels and air passages of the neck as a result of external pressure. There is a distinction between strangulation and choking, which is an internal obstruction of the airway. There is a misperception that strangulation is always fatal, and patients will often describe a “choking” episode following nonfatal strangulation.
Strangulation and Domestic Violence
Strangulation has been identified as one of the most lethal forms of domestic violence. It is one of the best predictors for subsequent homicide. Prior strangulation increases the odds of strangulation homicide by more than seven times.1 For perpetrators, strangulation is the ultimate form of power and control. However, because there are often no visible injuries, patients, physicians, and law enforcement often minimize the possible health consequences of reported strangulation.
Pathophysiology
The vasculature of the neck is relatively unprotected and vulnerable to injury and vascular occlusion. The application of 4.4 pounds of pressure to the jugular veins causes venous outflow obstruction from the brain and thus stagnant hypoxia. Eleven pounds of pressure to the carotid arteries can cause loss of consciousness in approximately 10 seconds. Compression of the trachea requires significantly more force: 33 pounds of pressure for occlusion and 35 pounds to fracture tracheal cartilage.2
Strangulation can be fatal in as little as four to five minutes. Mechanisms in addition to hypoxia due to vascular occlusion have been proposed. Pressure on the carotid body may cause bradycardia and subsequent cardiac arrest. Delayed mortality may be caused by carotid artery dissection, aspiration, postobstructive pulmonary edema, acute respiratory distress syndrome, or tracheal injury.
In domestic violence and sexual assault cases, manual strangulation (with hands or other body parts such as a knee) is most common. Ligature strangulation is significantly less common but more likely to result in visible injuries.
Clinical Findings
Frequently, strangulation does not result in visible physical findings.3 The lack of obvious injury, along with the distraught mental state of these patients, often results in underevaluation. It is important to perform a thorough exam, as findings may be subtle and located in difficult to see areas such as the scalp, behind the ears, and inside the mouth.
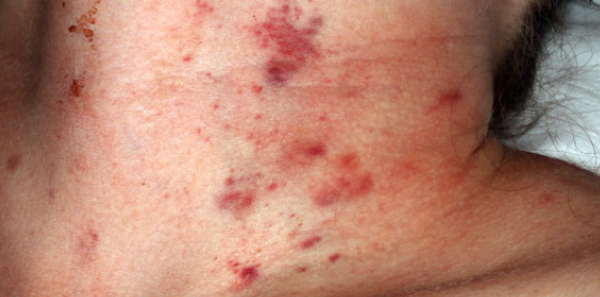
In the 50 percent of patients who have visible injuries, skin injuries are the most common. Faint bruises caused by the assailant’s fingertips, fingernail marks (sometimes self-inflicted), and petechiae may be seen. Subconjunctival hemorrhage may also occur.
Patients may have dysphagia and odynophagia. Voice changes are present in about half of strangulation cases; ask the patient if their voice sounds normal. Pain with movement of the tongue may indicate injury to the epiglottis. Although uncommon, hyoid fracture or tracheal cartilage fractures may result in crepitus followed by rapid airway obstruction.
Patients who have been strangled may present with pulmonary complaints, which are often mistakenly attributed to hyperventilation. Aspiration or postobstructive pulmonary edema may result in tachypnea and hypoxia.
Occlusion of or injury to one carotid artery may cause neurological deficits on the contralateral side. These include changes in vision, ptosis, facial droop, and unilateral weakness.4 If strangulation results in hypoxia, patients may have mental status changes and incontinence. Death has resulted days after strangulation due to hypoxic encephalopathy.
Miscarriage may also occur due to fetal hypoxia.3
Evaluation and Management
There is a paucity of evidence regarding the evaluation and management of patients who have been strangled. As pulse oximetry is rapid and noninvasive, it is universally recommended. Radiographs of the neck and cervical spine may reveal subcutaneous air, tracheal deviation, or hyoid fracture. However, CT is more sensitive for soft tissue injury, and CT angiography is indicated if vascular injury is suspected.
As symptoms may be delayed in onset, many experts recommend observation of strangulation patients with visible bruising, loss of consciousness, petechiae, or incontinence. Patients with reliable home monitoring and no apparent injuries may be discharged with careful instructions.5
Case Resolution
CT angiography shows soft tissue swelling but no vascular injury. The patient is hospitalized by the trauma service for observation. The local organization for victims of domestic violence is contacted to assist with safety planning prior to hospital discharge.
Dr. Riviello is chair of emergency medicine at Crozer-Keystone Health System and medical director of the Philadelphia Sexual Assault Response Center.
Dr. Rozzi is an emergency physician, director of the Forensic Examiner Team at WellSpan York Hospital in York, Pennsylvania, and chair of the Forensic Section of ACEP.
References
- Glass N, Laughon K, Campbell J, et al. Non-fatal strangulation is an important risk factor for homicide of women. J Emerg Med. 2008;35(3):329-335.
- McCance KL, Heuther SE. Pathophysiology. 6th ed. Maryland Heights, Mo: Mosby Elsevier; 2010.
- Strack GB, McClane GE, Hawley DA. A review of 300 attempted strangulation cases. Part 1: criminal legal issues. J Emerg Med. 2001;21(3):303-309.
- Stapczynski S. Strangulation injuries. Emerg Med Rep. 2010;31(17):193-203.
- Green W. Strangulation. In: Riviello RJ, Rozzi HV, eds. Evaluation and Management of the Sexually Assaulted or Sexually Abused Patient. 2nd ed. Dallas, Tex: American College of Emergency Physicians; 2014.
Pages: 1 2 | Multi-Page




2 Responses to “How to Evaluate Strangulation”
November 29, 2019
Bernd RaftlCan strangulation result in neck cancer
December 30, 2019
Ralph RivielloNot that I have seen in the medical literature.