
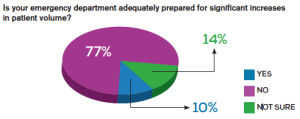
An online poll of emergency physicians conducted by ACEP showed that 86 percent of respondents expect emergency department visits to rise over the next three years. This could be due, in part, to the Jan. 1, 2014, implementation of the Affordable Care Act (ACA). Additionally, 77 percent reported that their EDs are not equipped for such significant increases. (You can view the complete poll results at http://newsroom.acep.org/ACEP-Emergency-Visits-Up-Since-Implementation-of-ACA.)
Explore This Issue
ACEP Now: Vol 33 – No 07 – July 2014“We conducted the poll to be sure that emergency departments had an understanding of future needs and that they will have the resources to meet the demand,” said Alex M. Rosenau, DO, FACEP, president of ACEP and senior vice chair of the department of emergency medicine at Lehigh Valley Health Network in Allentown, Pennsylvania.
The Issues at Hand
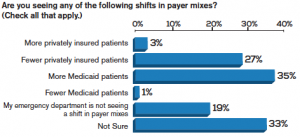
Although more Americans now have health care coverage, being covered doesn’t necessarily guarantee access. “Some people will have difficulty finding a primary care physician [PCP] because many have full schedules,” Dr. Rosenau said. “A delay in addressing chronic care can lead to acute emergencies.” Medicaid patients also commonly present to the ED because many PCPs, specialists, and urgent care centers typically don’t accept them due to low reimbursement. In fact, according to the poll, more than 35 percent of respondents are now seeing more Medicaid patients.
By 2020 there may be a shortage of up to 91,500 physicians; about half of these will be PCPs.1 The projected number of physicians will be insufficient to meet the needs of an aging population requiring more care. One factor creating this problem, Dr. Rosenau said, is that “the number of graduate medical education slots has been frozen for almost two decades.”
ACEP’s poll should be viewed as an alarm and a call to action. —Alex M. Rosenau, DO, FACEP, ACEP President
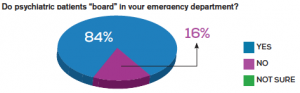
Care of patients with acute psychiatric illness is another growing problem. In the poll, 84 percent of respondents reported that these patients linger for days in the ED, waiting for a hospital bed—which clogs the ED system. “This is cruel and can lead to violent episodes,” Dr. Rosenau said. This occurs, in part, because few psychiatrists accept Medicaid or private insurance.
According to Michael J. Gerardi, MD, FACEP, President-Elect of ACEP, senior vice president of Emergency Medical Associates, and director of pediatric emergency medicine at Morristown Medical Center in Morristown, New Jersey, many more psychiatric patients could go home if more acute care options, such as intensive outpatient programs, were available. In addition, he said, “Physicians are hesitant to discharge many patients who would be fine as an outpatient due to liability concerns.”
To resolve these issues, Dr. Rosenau and Dr. Gerardi advise:
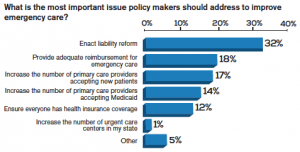
- Enacting liability reform (which the poll ranked as the most important solution to improving emergency care)
- Urging the government to increase the number of paid slots for physician training
- Enticing psychiatrists to see more patients by increasing Medicaid rates to Medicare rates
- Using telemedicine to increase access to psychiatrists who have inadequate availability due to manpower shortages and limited insurance/federal/state program participation
- Increasing the number of intensive outpatient treatment centers and programs
- Increasing inpatient capacity
- Addressing unfunded mandates, such as EMTALA
Action Needed
Armed with the poll’s results, Dr. Rosenau and Dr. Gerardi urge ACEP members to share the information with individuals who have decision-making power (eg, state and federal legislators, medical societies, and hospital administrators). For an even greater impact, Dr. Rosenau and Dr. Gerardi recommend becoming involved in local politics or supporting your state’s medical society chapter.
Dr. Gerardi said that congressional representatives are willing to listen because emergency physicians care for many of their constituents. “Stories illustrating the data win the day inside the halls of Congress,” he said. “If you can’t visit your congressman, share your stories with ACEP, and we will take them to Washington, D.C., for you.”
Stories illustrating the data win the day inside the halls of Congress. —Michael J. Gerardi, MD, FACEP, ACEP President-Elect
ACEP is urging Congress to make a firm commitment to emergency medicine patients by holding a hearing to examine whether additional strains are occurring in the ED safety net as a consequence of ACA.
Future Outlook
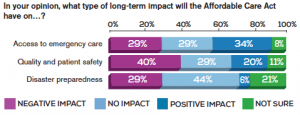
Dr. Rosenau maintains that all U.S. citizens deserve health care coverage. Of those polled, 34 percent believed that the ACA will have a positive impact on access to emergency care in the long term.
But in the near and middle term, there is a danger that there won’t be adequate infrastructure to ensure adequate care. “We need Congress to act,” Dr. Rosenau said. “Many politicians think emergency medicine contributes to the high cost of medical care, but ultimately, it is a valuable service for a reasonable price for 136 million people per year.”
“ACEP’s poll should be viewed as an alarm and a call to action,” Dr. Rosenau concluded.
Karen Appold is a writer in Pennsylvania
Reference
Pages: 1 2 | Multi-Page




2 Responses to “Emergency Department Visits On the Rise”
December 3, 2014
Emergency Department Visits Hit Record High, With More Cases Requiring Urgent Treatment - ACEP Now[…] the Affordable Care Act (ACA), there is already evidence that emergency visits are on the rise now. Nearly half of emergency physicians responding to an ACEP poll in April reported a rise in emergency… Nearly 90 percent expected emergency visits to increase over the next three years, and more than […]
May 6, 2015
Emergency Department Visits Increasing, ACEP Poll Shows - ACEP Now[…] are going up, according to a new poll [PDF]. This represents a significant increase from just one year ago when less than half reported increases. Rather than trying to keep people out of emergency […]