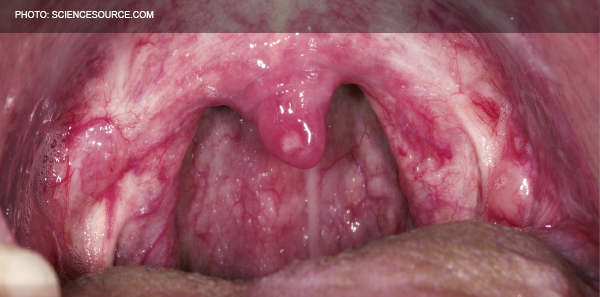
In addition to our nominal business of handling true medical emergencies, typical emergency departments also provide care for many patients with ambulatory medical complaints. Whether these patients present due to anxiety over the nature of their condition, to alleviate suffering, or for sheer convenience, these non-emergencies may prove just as challenging. Acute pharyngitis, for example, represents more than 1 million visits annually to US emergency departments. This presenting complaint rarely requires or benefits from antibiotics, yet the desire to provide our patients with at least some token of relief is frequently strong enough to overcome the rationality of antibiotic stewardship. Estimated appropriate prescribing rates for pharyngitis, accounting for group A strep prevalence, are 10 percent to 20 percent, but antibiotics are prescribed in roughly 60 percent of cases.1
Explore This Issue
ACEP Now: Vol 36 – No 06 – June 2017What alternative might we have to our ill-conceived antibiotic prescriptions? How about systemic steroids?
It follows logically that if pharyngitis is associated with inflammation of the pharynx, perhaps strong anti-inflammatory immunoregulation might prove beneficial. We have seen our otolaryngology colleagues prescribe steroids postoperatively for edema and pain. Should we use them for uncomplicated pharyngitis in our ambulatory population?
Examining Steroid Use for Sore Throats
In fact, it’s a little facetious to even ask such questions, considering many physicians already routinely incorporate consideration for oral steroids into their treatment options for pharyngitis. Most frequently, these are given as a one-time dose, either oral or intramuscularly, of dexamethasone or prednisone. However, for such a common treatment, the evidence is weaker than one may expect.
The largest examination of systemic steroids for acute pharyngitis comes in the form of a Cochrane Review.2 Unfortunately, despite being the largest review, the evidence base consists of a mere eight studies and 743 patients. These studies include patients from all over the globe; evaluate varying doses, types, and routes of steroids; mostly include adjuvant antibiotics; and measure all manner of differing outcomes. Despite the mostly consistent results favoring steroids, the only reliable conclusion is the need for a more robust trial.
This leads us to the 2017 publication in JAMA of the Treatment Options without Antibiotics for Sore Throat (TOAST) trial.3 This trial randomized 565 patients with acute sore throat to either 10 of oral dexamethasone or identical placebo. Patients were eligible for enrollment provided clinicians did not prescribe immediate antibiotics, but clinicians were allowed to provide antibiotics for delayed use if symptoms did not improve.
A long story made short, this is a negative trial. There was no statistically significant difference in complete symptom resolution at the 24-hour primary outcome. The difference between groups, 22.6 percent resolution in the dexamethasone group versus 17.7 percent resolution in placebo, was much smaller than expected based on the results from prior trials in which nearly three times as many patients in the dexamethasone group experienced symptomatic relief.
No long story can truly be made short. Anecdotally, most clinicians reading these data found they reinforced their preexisting opinion, whether they felt steroids were beneficial or not. For those clinicians who have been using dexamethasone with positive effects in their practice, these data are viewed through the lens of their experience and the prior research. In this view, the statistically negative result is a feature of inadequate sample size, and all the secondary outcomes consistently tilt toward dexamethasone. Symptom relief at 48 hours favored dexamethasone by 8.7 percent, a number needed to treat of 12, and almost all the quality-of-life and resource utilization outcomes likewise show small beneficial effects.
Oral dexamethasone is universally inexpensive, and the preponderance of evidence suggests it’s helpful, so why is this potentially controversial? Why were any clinicians taking the opposing viewpoint that this treatment should not be routinely adopted? This is likely because the intervention has likely been downgraded from “harmless” to “mostly harmless.”
The Risks of Steroids
In certain patients, the deleterious effects of systemic steroids are obvious and avoidable. However, we expect most healthy young patients to tolerate short low-dose courses of steroids without ill effects. A recent publication in BMJ, unfortunately, suggests serious adverse outcomes are substantially more common from steroid exposures.4
These authors reviewed a commercial insurance database and a final cohort of more than 1.5 million patients to examine for associations between short-course steroid exposure and sepsis, venous thromboembolism, and fractures. As compared with patients without exposure to steroids, patients prescribed steroids had roughly double the risk for sepsis, a 60 percent increase for venous thromboembolism, and a 25 percent increase for fractures in the five- to 90-day period following exposure. The numbers needed to harm for each of these conditions range from approximately 3,000 for sepsis to 800 for fractures. The harms were not equally distributed across ages, with lower risks for younger patients and increased risks for those older. However, the risks remained substantially increased. These increases in adverse events also held true for short courses and low doses of steroids.
So where does that leave us? Steroids probably do provide some benefit in symptomatic relief of pain from acute pharyngitis but not to the magnitude reflected in earlier trials. At the same time, this treatment is probably not quite as risk-free as previously thought. Ideally, evidence from trials would be robust enough to show signals of which patients were more likely to benefit from steroids, but with just a few hundred in each treatment group, nothing reliable can be gleaned. Ultimately, we will have to wade into a realm of some uncertainty and make individualized assessments of the value of potential benefit as well as of the likelihood of benefit and rare but important harms.
References
- Barnett ML, Linder JA. Antibiotic prescribing to adults with sore throat in the United States, 1997-2010. JAMA Intern Med. 2014;174(1):138-140.
- Hayward G, Thompson MJ, Perera R, et al. Corticosteroids as standalone or add-on treatment for sore throat. Cochrane Database Syst Rev. 2012;10:CD008268.
- Hayward GN, Hay AD, Moore MV, et al. Effect of oral dexamethasone without immediate antibiotics vs placebo on acute sore throat in adults: a randomized clinical trial. JAMA. 2017;317(15):1535-1543.
- Waljee AK, Rogers MA, Lin P, et al. Short term use of oral corticosteroids and related harms among adults in the United States: population based cohort study. BMJ. 2017;357:j1415.
Pages: 1 2 3 | Multi-Page






No Responses to “Is Dexamethasone Helpful for Treating Pharyngitis?”