During the COVID-19 pandemic, there has been a documented decline in emergency department visits for medical and traumatic conditions, myocardial infarctions, stroke, and hyperglycemic crises.1–3 Four in 10 adults have deferred care for fear of contracting the novel coronavirus, which complicates a patient’s disease course and places them in a higher-mortality cohort.4 A recent survey conducted by ACEP found that 80 percent of respondents were concerned about contracting COVID-19 from another patient or visitor in the emergency department, and 29 percent have actively delayed or avoided seeking medical care due to concerns about contracting COVID-19.5 Another survey found that, regarding non-COVID-19-related complaints, 59 percent of respondents were unlikely to utilize emergency care, with an additional 20 percent of respondents who “don’t know.”6
We present a case study of a patient whose fear of contracting COVID-19 led to significant morbidity.
Case Report
A 79-year-old African American male presented to the emergency department with a two-week history of right leg swelling and darkness of his right second toe. He denied any history of trauma, pain, or erythema. The patient did not report any systemic symptoms, including fever, malaise, or weakness. His medical history was notable for hypertension and ulcerative colitis, the latter of which was managed by infliximab. The patient reported smoking 0.5 packs per day. He had delayed seeking medical treatment for two weeks due to fear of COVID-19.
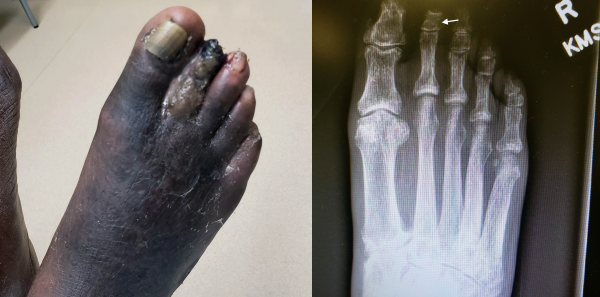
On examination, the patient appeared well, with normal speech and mental status. Vital signs were normal. Cardiac, pulmonary, and abdominal exams were unremarkable. Examination of the right leg demonstrated moderate edema of the calf. Moderate erythema and edema were seen on the dorsum of the right foot. Right dorsalis pedis and posterior tibial pulses were not palpable. The right second toe was notable for gangrene, purulence, and an absent distal phalanx (see Figure 1).
Laboratory studies included a glucose of 103 mg/dL, hemoglobin of 12.3 g/dL, and erythrocyte sedimentation rate (ESR) of 100 mm/h. A plain radiograph of the right foot showed osteomyelitis of the second middle phalanx (see Figure 2). Ultrasound of the right lower extremity revealed an occlusion extending from the right superficial femoral artery through the popliteal artery. No deep vein thrombosis was found.
Empiric antibiotic treatment with intravenous vancomycin and piperacillin/tazobactam was initiated in the emergency department. The patient was admitted to the hospital and received consultations from infectious disease, podiatry, and vascular surgery specialists. On hospital Day 3, he underwent right iliofemoral endarterectomy with bovine patch angioplasty, right proximal superficial femoral artery endarterectomy, and right femoral artery to tibial artery saphenous vein bypass. On hospital Day 7, he underwent a right second digit amputation and flap. He was discharged home after 11 days in good condition.
Discussion
Critical limb ischemia (CLI) is the most advanced stage of peripheral artery disease (PAD) and is associated with significant morbidity and mortality.7,8 A 2019 report estimates the U.S. prevalence of CLI to be 1.3 percent in patients above the age of 40 (2 million people), while PAD affects more than 200 million people worldwide.8,9
The “5 P’s” of CLI are pain, pulselessness, pallor, paresthesia, and paralysis. These features are found in 48 to 90 percent of the acute presentations of limb ischemia.10,11 Rarely, progression to severe ischemia leads to ulceration of the digits of the foot (8.5 percent of cases) and frank gangrene (5.2 percent of cases).7,11
Smoking and diabetes are the most significant risk factors of CLI, but others include African American race, male sex, being more than 40 years old, hypertension, dyslipidemia, elevated C-reactive protein, hypercoagulable states, hyperhomocysteinemia, chronic renal insufficiency, and history of cardiovascular disease.7,9,10 The one-year mortality in CLI patients with gangrene is 33.2 percent, which jumps to 68.5 percent over four years.12
The COVID-19 pandemic has resulted in fear of seeking health care, which can contribute to preventable morbidity and mortality.
This case describes a significant delay in seeking medical care due to fear of COVID-19, resulting in worsening osteomyelitis and gangrene and ultimately requiring multiple surgical interventions and prolonged antibiotic therapy. Although our patient had risk factors for PAD, the development of severe and life-threatening CLI potentially could have been mitigated with early intervention.
Many local and national organizations are working to educate the public about seeking appropriate medical care.13–17 Continued patient education at the local and national level is necessary to ensure timely and appropriate medical treatment.



Mr. Asarpota is a medical student; Dr. Wyss is chief resident, emergency medicine; and Dr. Marco is professor of emergency medicine at the Wright State University Boonshoft School of Medicine in Dayton, Ohio.
References
- Masroor S. Collateral damage of COVID-19 pandemic: delayed medical care. J Card Surg. 2020;35(6):1345-1347.
- Messac L, Knopov A, Horton M. Delayed care-seeking for non-COVID illnesses in Rhode Island. R I Med J. 2020;103(4):10-11.
- Lange SJ, Ritchey MD, Goodman AB, et al. Potential indirect effects of the COVID-19 pandemic on use of emergency departments for acute life-threatening conditions — United States, January–May 2020. MMWR Morb Mortal Wkly Rep. 2020;69(25):795-800.
- Czeisler MÉ, Marynak K, Clarke KEN, et al. Delay or avoidance of medical care because of COVID-19–related concerns—United States, June 2020. MMWR Morb Mortal Wkly Rep. 2020;69(36):1250-1257.
- Public poll: emergency care concerns amidst COVID-19. ACEP website. Accessed May 29, 2020.
- National tracking poll #2004100 April 29–30, 2020. Morning Consult website. Accessed May 22, 2020.
- Fabiani I, Calogero E, Pugliese NR, et al. Critical limb ischemia: a practical up-to-date review. Angiology. 2018;69(6):465-474.
- Duff S, Mafilios MS, Bhounsule P, et al. The burden of critical limb ischemia: a review of recent literature. Vasc Health Risk Manag. 2019;15:187-208.
- Fowkes FGR, Rudan D, Rudan I, et al. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: a systematic review and analysis. Lancet. 2013;382(9901):1329-1340.
- Norgren L, Hiatt WR, Dormandy JA, et all. Inter-society consensus for the management of peripheral arterial disease (TASC II). J Vasc Surg. 2007;45 Suppl S:S5-S67.
- Zarins CK. A comparison of recombinant urokinase with vascular surgery for acute arterial occlusion of the legs. N Engl J Med. 1998;339(8):564; author reply 564-565.
- Mustapha JA, Katzen BT, Neville RF, et al. Determinants of long-term outcomes and costs in the management of critical limb ischemia: a population-based cohort study. J Am Heart Assoc. 2018;7(16): e009724.
- Wong LE, Hawkins JE, Langness S, et al. Where are all the patients? Addressing Covid-19 fear to encourage sick patients to seek emergency care. NEJM Catal. 2020. doi: 10.1056/CAT.20.0193.
- COVID-19: know when to go. ACEP website. Accessed May 29, 2020.
- Hsieh P. Do not delay urgent medical care due to the COVID-19 coronavirus pandemic. Forbes website. Accessed May 29, 2020.
- Washington State Department of Health. Heart attack and stroke don’t stop for COVID-19. Medium website. Accessed May 29, 2020.
- American Heart Association urges patients to quickly call 911 for chest pain or heart symptoms. American Heart Association website. Accessed May 29, 2020.
Pages: 1 2 3 | Multi-Page




One Response to “Case Report: Fear of COVID-19 Leads to Gangrene”
February 14, 2021
Thomas B, MDI saw a similar case recently. Our patient was diagnosed with Covid-19 and he dutifully remained in quarantine as instructed while his foot became necrotic and progressed to sepsis. He was critically ill when we flew him out from our critical access hospital.