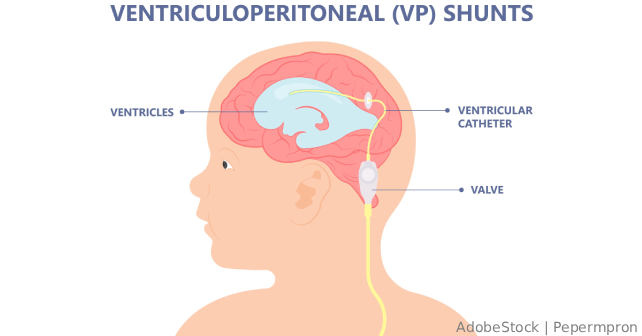
A 3-year-old girl with a history of prematurity, hydrocephalus status post ventriculoperitoneal (VP) shunt at four months, and developmental delay was brought to the emergency department (ED) for one day of fever, abdominal pain, vomiting, and lethargy. Vital signs were T 98.2°F, HR 64, RR 19, weight 9.98 kg, SpO₂ 100%. The exam documented an alert, awake child in mild distress who was “averbal at baseline,” a palpable right-sided shunt, no meningismus, a soft non-tender abdomen, and “appropriate for age” interaction with normal strength and tone.
Explore This Issue
ACEP Now: March 2026Initial diagnostic evaluation included a shunt series showing intact tubing, a CT brain with no hydrocephalus and unchanged from prior imaging, and labs notable for Na 134 mEq/L, lactate 2.0, WBC 18, Hgb 12.4, and platelets 136. Blood and urine cultures were obtained. The medical decision making stated that the patient was treated with normal saline intravenous (IV) fluids, 4 mg ondansetron, and admitted to primary care physician at 0020 with a diagnosis of dehydration and vomiting.
During handoff to the floor, the patient’s mother reported six episodes of emesis, only three wet diapers in 24 hours (baseline six), and new crossing of the eyes. Exam showed HR 56, RR 18, BP 92/59, SpO₂ 98%, lethargy, bilateral esotropia, and generalized hypotonia. The patient was transferred to the pediatric intensive care unit, started on ceftriaxone and vancomycin, and neurosurgery was consulted. Shunt malfunction was considered unlikely because the valve pumped and refilled and CT ventricular size appeared stable, though a shunt tap was planned if symptoms progressed.
Overnight the patient had episodes of bradycardia, hypertension, decreased mental status, gaze deviation, vomiting, brief seizures, and head-grabbing. Repeat CT remained unchanged. She was treated with hypertonic saline and symptomatic medications. While in the operating room (OR) the next morning for a planned shunt revision, the patient unexpectedly spoke and requested pizza; the procedure was cancelled. Her condition declined the following day, and when she returned to the OR, her pupils were fixed and dilated. She was declared brain dead days later. Autopsy revealed global acute/subacute hypoxic-ischemic injury without infection. A defense verdict resulted, likely because the defense persuaded the jury that the patient’s sudden deterioration and death were caused by “status epilepticus” rather than a failure to perform neurosurgery. This provided a “proximate cause” for the death that was independent of the physician’s decisions regarding the shunt.
Issues and Key Points in Care
- Inconsistent Documentation of Baseline Function: The ED described the child as “averbal at baseline” while prior and subsequent notes showed she was bilingual. This discrepancy obscured recognition of an acute neurologic change, which should prompt concern for central nervous system pathology.
- Inadequate Vital Sign Documentation: The ED obtained no blood pressure and only one heart rate, which was bradycardic for age. Without serial measurements, evolving signs of Cushing’s triad could not be recognized. Staff may consider blood pressure measurement technically difficult or low-yield, but it is essential in any child with lethargy, vomiting, or a VP shunt.
- Medication Dosing Concern: She received 4 mg oral ondansetron despite a weight of 9.9 kg, exceeding the standard pediatric dose (0.15 mg/kg). This reflects inattention to weight-based dosing in mixed-age EDs.
- Discordant Neurologic Findings: ED documentation of normal tone contrasted with hypotonia two hours later. In children with developmental delay and/or VP shunts, tone can vary at baseline. Without knowing this, clinicians risk missing deterioration.
- Inappropriate Use of Hypertonic Saline: She was given 3 percent saline for a sodium of 134 mEq/L; this was not indicated. The effect was to unintentionally reduce intracranial pressure, producing transient improvement and contributing to false reassurance and delayed definitive management.
- Intermittent Shunt Obstruction: Her waxing and waning symptoms — vomiting, lethargy, gaze deviation, and bradycardia — are characteristic of intermittent shunt obstruction, a less common but well-described pattern of malfunction. Ventricular size may remain stable, and fluctuating symptoms can create false reassurance. Normal shunt refill and CT-measured ventricular size do not exclude obstruction, particularly in chronically shunted children. MRI provides superior assessment, and a normal CT cannot rule out malfunction in a symptomatic patient.
 Dr. Cohen is a dual board-certified expert in pediatric emergency medicine and emergency medicine with extensive experience in clinical practice, peer review, and medicolegal consultation.
Dr. Cohen is a dual board-certified expert in pediatric emergency medicine and emergency medicine with extensive experience in clinical practice, peer review, and medicolegal consultation.




No Responses to “Case Report: Failure To Diagnose Shunt Malfunction Results in Death”