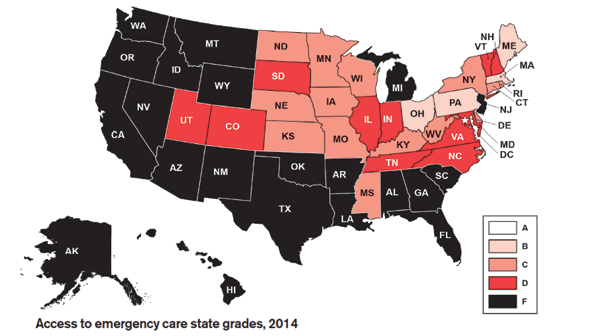
A near-failing grade for most states points to subpar conditions and policies for delivery of EM care, lack of support for hospitals, say ACEP leaders
Last month’s release of ACEP’s 2014 Report Card on Emergency Medicine was considered a wake-up call to the health-care system, revealing a lack of support for emergency patients and a deserving D+ overall grade. One category set off the fire alarm.
Explore This Issue
ACEP Now: Vol 33 – No 02 – February 2014Access to Emergency Care, which accounted for 30 percent of the overall grade and was weighted more heavily than the other four (Quality and Patient Safety, Medical Liability Environment, Public Health and Injury Prevention, and Disaster Preparedness) and showed that very few states get the support they need in terms of conditions and policies under which emergency care is being delivered. It received a grade nationwide of D-, and 22 states received an F.
Overall, this category hasn’t improved since the last time ACEP released the Report Card in 2009.
The Report Card measures conditions and policies under which emergency care is being delivered, not the quality of care provided by hospitals and emergency providers. Emergency physicians across the country, including ACEP President Alex M. Rosenau, DO, FACEP, say this category is crucial when it comes to improving the support for emergency department patients. ACEP is encouraging its members to talk with legislators and make them aware of deficiencies.
“Access is one of the most important parts of providing care to any type of patient,” Dr. Rosenau said. “If a patient can’t get in to see a physician and can’t get care, the best medicine in the world won’t mean anything.”
ACEP points out in the report that access to emergency care is both fundamental and complex. The College is urging news outlets to recognize that emergency departments are a vital part of the health care system in each community and region. They deliver emergency care day in and day out, and they serve as the health care safety net for anyone, insured or not, who cannot otherwise obtain timely health care services when needed. Access to emergency care is complex because the demand for emergency services often is related to the capacity of the broader health care system to deliver services.
Thus, measures of Access to Emergency Care must include elements that comprise that broader system. This category measures the availability of emergency care resources, such as numbers of emergency physicians, emergency departments, registered nurses, and trauma centers per person, along with proximity to Level I or II trauma centers, and the median time from arrival to departure from the emergency department. Because emergency department capacity is also a function of the broader health care system, the access category includes key measures of that system’s capacity, such as the availability of primary care, mental health care, and substance abuse treatment.
It also includes the numbers of available inpatient hospital beds, psychiatric beds, and designated pediatric specialty centers because greater capacity in those areas can alleviate crowding and boarding within emergency departments. Because one of the most commonly cited concerns in emergency departments across the country is the lack of access to on-call specialists, this category also includes measures of the total supply of commonly requested specialists, including neurosurgeons; orthopedists; hand surgeons; plastic surgeons; and ear, nose, and throat specialists.
“America’s grade for Access to Emergency Care was a near-failing D- because of declines in nearly every measure,” said Jon Mark Hirshon, MD, MPH, PhD, FACEP, the chair of the task force that directed development of the Report Card. “It reflects that hospitals are not getting the necessary support in order to provide effective and efficient emergency care. There were 19 more hospital closures in 2011, and psychiatric-care beds and hospital-inpatients beds have fallen significantly, despite increasing demand. People are increasingly reliant on emergency care, and primary care physicians are advising their patients to go to the emergency department after hours to receive complex diagnostic workups and to facilitate admissions for acutely ill patients.”
The Report Card includes several national recommendations, including requests to:
- Fund the Workforce Commission, as called for by the Affordable Care Act (ACA), to investigate shortages of physicians, nurses, and other health care professionals.
- Pass the Health Care Safety Net Enhancement Act of 2013, H.R. 36, introduced by Rep. Charlie Dent (R-Pa) and the companion legislation, S. 961, introduced by Sen. Roy Blunt (R-Mo). This legislation would provide limited-liability protections to (emergency and on-call) physicians who perform the services mandated by the federal EMTALA law, which requires emergency patients be screened, diagnosed, and treated regardless of their insurance status or ability to pay.
- Fund pilot programs, provided for in the ACA, to design, implement, and evaluate innovative models of regionalized, comprehensive, and accountable emergency care and trauma systems.
- Support and fund the mission of the Emergency Care Coordination Center at Department of Health and Human Services to create an emergency-care system that is patient and community-centered, integrated into the broader health-care system, high quality, and prepared to respond in times of public health emergencies.
- Withhold federal funds to states that do not support key safety legislation, such as motorcycle helmet laws and .08 blood alcohol content laws.
- Fund graduate medical education programs that support emergency care, especially those related to addressing physician shortages in disadvantaged and rural areas.
- Support efforts to fund emergency care research by the new Office of Emergency Care Research under the National Institutes of Health.
- Hold a hearing to examine whether additional strains are occurring in the emergency department safety net as a consequence of the ACA.
For a full list of recommendations, to see state grades, and to see how you can help, go to www.emreportcard.org.
Pages: 1 2 3 | Multi-Page






No Responses to “ACEP’s 2014 Report Card on Emergency Medicine Reveals Major Access-to-Care Deficit”