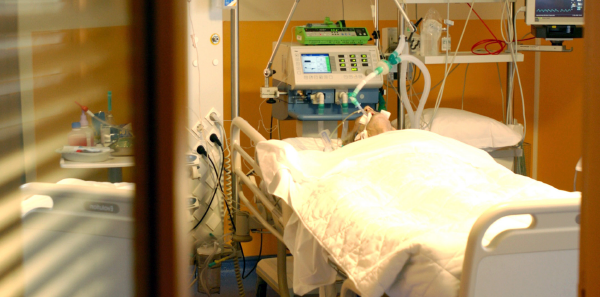
During a busy ED shift, you are called to the resuscitation bay to evaluate an 86-year-old woman found by EMS. She was found alone and unconscious and was intubated in the field for airway protection. Your workup in the emergency department reveals a large ascending aortic dissection that, per the surgeon, is likely fatal without emergent surgery. Soon, her family arrives and informs your team that the patient had previously requested “do not resuscitate” and “do not intubate” (DNI) directives and would not want invasive surgery. After speaking with the surgeons, the family requests that the patient be taken off the ventilator in keeping with the patient’s wishes. What are your next steps?
Explore This Issue
ACEP Now: Vol 40 – No 08 – August 2021As emergency physicians, intubating patients is an essential component of our job. We are well-versed in the procedures, medications, and equipment available to swiftly and safely secure a patient’s airway. But sometimes, as we gather more information, we will be asked to perform the opposite: to assist with terminal extubation. Although this decision may seem daunting, under the correct circumstances, terminal extubation is an important skill that, according to the American Board of Emergency Medicine Model of the Clinical Practice of Emergency Medicine, should be within the scope of practice of all emergency medicine clinicians.1
Terminal extubation should be considered if the patient has an advance directive specifying DNI or their decision maker clearly states that intubation is not consistent with the patient’s established wishes. Specific circumstances in which intubation may occur, then need to be reversed include cases in which a patient arrives actively coding with limited information, cannot communicate and has no decision maker readily available, arrives prior to discovering medical history that worsens prognosis, or is discovered to have a new fatal diagnosis for which intubation is deemed nonbeneficial.
In the most straightforward scenarios, there is a clear decision maker or written documentation requesting DNI and no prohibitive time nor resource constraints in the emergency department. One simple communication tip to help decision makers with this difficult decision is to refocus the discussion on the patient and their wishes: “Tell me about [patient name]. If [patient name] could talk with us right now, what do you think they would tell us to do?” If intubation is not part of the patient’s goals of care, the emergency physician should move forward with terminal extubation.
Once the decision to proceed is made and appropriate team members have been mobilized, emergency physicians should consider the timing of the extubation process. Depending on the circumstances, it may be prudent to await the arrival of other family members.
Terminal extubation may also be an appropriate option if a physician concludes aggressive care is nonbeneficial or not appropriate. For example, during the COVID-19 pandemic, with limited life-sustaining equipment (ventilators, extracorporeal membrane oxygenation) and limited ICU bed availability, some emergency physicians were asked to terminally extubate moribund patients. We acknowledge that there will also be circumstances in which the decision to terminally extubate is better made as an inpatient, including patients who lack a clear decision maker, a code status that cannot be clearly elucidated, an unclear prognosis, or prohibitive resource or time constraints in the emergency department. Despite this, we believe that terminal extubation in the emergency department is appropriate in some situations and therefore an important skill set for emergency physicians.
Preparation
Appropriate preparation for terminal extubation is a critical, often overlooked step to ensure a smooth process for all parties. We must educate and prepare staff about this procedure before the need acutely arises. Consider identifying nurses in advance who can have reduced assignments while they assist with patients undergoing terminal extubation. If available, resources to offer spiritual and emotional support are especially valuable. Many inpatient palliative care teams have a dedicated chaplain and social worker who are specifically trained for these scenarios, and their expertise should be utilized.
Once the decision to proceed is made and appropriate team members have been mobilized, emergency physicians should consider the timing of the extubation process. Depending on the circumstances, it may be prudent to await the arrival of other family members. Understanding the hospital’s visitation policy is also important, as the inability to allow certain family members to visit may affect the decision of when to extubate. For example, some adult emergency departments do not allow visitors under age 18, which might push family to instead pursue extubation as an inpatient, where visitation rules are less stringent.
Once family is gathered, it is essential to set expectations and provide anticipatory guidance regarding what might happen and what symptoms the patient might experience. One common question from family members is how long the process will take. Although this can vary, studies indicate median time to death after ventilatory withdrawal for terminal extubation is 0.9 hours, and the vast majority die within 10 hours.2 As physicians, we should clarify this uncertainty in advance. “I wish I knew exactly how long this might take. It usually happens within 10 hours, but I can’t give you an exact answer. I can promise we will do our best to make your loved one comfortable.”
After communicating with the family, identify an appropriate room for the extubation to occur. Ideally, this space should be private, quiet, and spacious enough to accommodate family members; some emergency departments have had success in utilizing observation or “flex” rooms for this purpose. With the assistance of the registered nurse and patient technicians, take a moment to set up the room by muting monitors and providing water, chairs, tissues, and blankets for loved ones.
Extubation Management and Disposition
Once the patient and family are ready, the emergency physician should shift focus to the medical management of extubation. In anticipation of common post-extubation symptoms, emergency clinicians should have push-dose medications readily available, including opioids for pain or dyspnea, benzodiazepines for anxiety, glycopyrrolate for terminal secretions, and steroids or nebulized epinephrine for stridor.3 In addition to medications, a towel and suction are helpful to manage excess secretions on the endotracheal tube and in the oropharynx. Depending on the patient’s current respiratory status, we may opt for either direct terminal extubation or a terminal wean in which ventilatory settings are reduced in a stepwise fashion every few minutes to provide a more gradual decrease in respiratory support.4 The respiratory therapist may be able to assist with this process. After assembling the multidisciplinary team, communicating with family, and preparing the room and medications, the extubation itself may often feel like the easiest part of this process.
Following extubation, it is important to consider potential dispositions if time to death is prolonged. We should consider whether patient needs might best be met in inpatient hospice, home hospice, or the acute care hospital. Coordinating with the case manager, social worker, or chaplain may help elucidate which options are most appropriate. If available, we should collaborate with existing palliative care teams to utilize appropriate resources. These teams can provide guidance and support, especially for physicians new to the process.
Systems-Level Considerations
Organizing terminal extubation in the emergency department may seem overwhelming, especially if there are no existing systems in place to help guide busy physicians through these steps. To mitigate this barrier, emergency departments should pre-establish protocols and order sets to streamline this process for clinicians. These protocols can help identify patients who are good candidates for ED extubation and outline clear steps forward, including who to call and what resources are available.
As part of these protocols, it is prudent to pre-identify private care rooms/flex rooms in our emergency departments that may be closer to the nursing station, quieter, and adaptable to larger families. Emergency departments should also create order sets with common medications and dosing recommendations for end-of-life issues. They should also address how to set up the room (eg, turning off the monitors and providing chairs). These order sets significantly reduce cognitive burden and improve consistency, which is especially important given wide variations in comfort levels of physicians carrying out this procedure.
If possible, offer training on terminal extubation to all ED staff and identify champions from nursing, care coordination, social work, and chaplaincy as well as physicians, nurse practitioners, and physician assistants who can help to integrate and improve this process. Finally, we should anticipate staff and resource constraints and proactively address common challenges (eg, chaplain availability during nights or weekends, feasibility concerns during peak hours, etc.). Our palliative care colleagues may be able to provide us support during these times. Ideally, multidisciplinary huddles should occur after each terminal extubation to improve the experience through quality improvement initiatives and build team resilience. A team-based approach can help make this complex process easier for patients, families, and hospital staff.
Conclusions
Although performing terminal extubation in the emergency department presents unique challenges, it is likely that all emergency physicians will encounter appropriate scenarios for terminal extubation. By utilizing multidisciplinary teams, providing clear communication to families, creating systemwide protocols and order sets, and continually assessing these protocols, we can streamline this process and provide better care for our patients. It is our hope that this guidance will help you to carry out this important procedure for appropriate patients in the emergency department while avoiding common pitfalls.
 Dr. Hosain is third-year emergency medicine resident at Yale New Haven Hospital in Connecticut.
Dr. Hosain is third-year emergency medicine resident at Yale New Haven Hospital in Connecticut.
 Dr. Wallingford is a fellow physician in hospice and palliative medicine in the department of internal medicine at Dell Medical School at the University of Texas at Austin.
Dr. Wallingford is a fellow physician in hospice and palliative medicine in the department of internal medicine at Dell Medical School at the University of Texas at Austin.
 Dr. Jubanyik is associate professor of emergency medicine at Yale University School of Medicine.
Dr. Jubanyik is associate professor of emergency medicine at Yale University School of Medicine.
References
- Counselman FL, Babu K, Edens MA, et al. The 2016 model of the clinical practice of emergency medicine. J Emerg Med. 2017;52(6):846-849.
- Huynh TN, Walling AM, Le TX, et al. Factors associated with palliative withdrawal of mechanical ventilation and time to death after withdrawal. J Palliat Med, 2013;16(11):1368-1374.
- Cassone M, Stoltzfus G, Melnychuk E. Terminal extubation in the ED: palliative care in EM. Emergency Medicine Residents’ Association website. Accessed July 9, 2021.
- Marr L, Weissman DE. Withdrawal of ventilatory support from the dying adult patient. J Supp Onc. 2004;2(3):283-288.
Pages: 1 2 3 4 | Multi-Page


No Responses to “A Patient- and Family-Focused Approach to Terminal Extubation”