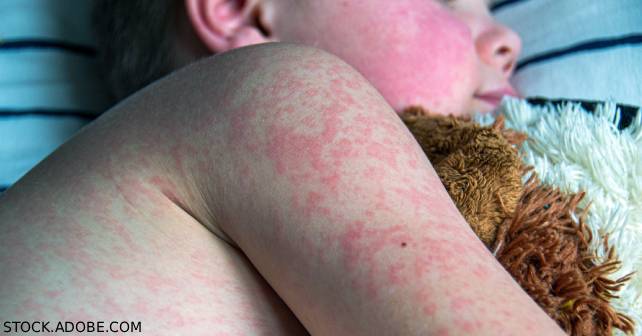
Acute measles in the emergency department, once a rarity, is now a reality. This means it is time for all departments to dust off old protocols for its immediate treatment and subsequent management. The good news — and the bad — is that little has changed over the intervening decades of measles eradication. However, the quiver of effective treatments, from back in the days when universal vaccination had not yet taken root, remains fairly empty.
Explore This Issue
ACEP Now: March 2026The first, and simplest, concern following identification of acute measles in the emergency department is isolation. The most cited basic reproduction number for measles virus is in the 12 to 18 range, although variability exists beyond that general estimate. This reproduction number represents a rough proxy for the practical infectivity of a virus, and the measles virus shows dramatically greater transmission than its common comparators.
For example, SARS-CoV-2, the world-altering scourge, carried R0 estimates of generally between 2 to 4, while varicella is approximately 9, mumps and rubella around 7, and poliomyelitis around 5. Isolation in a negative-pressure room is necessary to minimize risk of transmission, accompanied by fit-tested respiratory masks such as N95 or P2.
For the vast majority of identified measles cases, nonspecific supportive care will be the only necessary treatment. For ambulatory patients not displaying any signs of dehydration, pneumonia, or encephalitis, no immediate treatment is universally indicated. The most commonly cited treatment for acute measles, if any is deemed appropriate, is vitamin A.
High-quality randomized controlled trial evidence exists regarding the benefit of vitamin A supplementation in measles, with the effect most prominently seen in patients with vitamin A deficiency. Most children and adults in the United States should not be expected to be suffering from vitamin A deficiency, in contrast to those living in resource-limited countries. Due to the beneficial effects seen, however, the American Academy of Pediatrics (AAP) and the Centers for Disease Control and Prevention (CDC) offer strong recommendations to provide vitamin A in patients being hospitalized for severe measles, regardless of suspected nutritional status.
Useful evidence to support vitamin A in non-severe measles is substantially less robust, but supplementation is unlikely to be harmful at the recommended doses. Excessive vitamin A can result in a range of toxic effects, and should therefore be limited to the recommended doses:
- 50,000 IU for infants younger than 6 months of age
- 100,000 IU for infants 6–11 months of age
- 200,000 IU for children 12 months of age and older
An initial dose can be provided immediately upon diagnosis, and the treatment course concludes with a second dose repeated the following day.
Cod liver oil supplementation should be discouraged in lieu of the recommended dosing regimen from the AAP and CDC. Although one tablespoon of cod liver oil ought to contain 13,600 IU of vitamin A, the exact amount may vary by preparation, and continued use may contribute to aforementioned vitamin A toxicity.
No additional validated treatments for measles exist, neither antibiotics nor antivirals are presently shown to be useful for the outpatient management of measles. In hospitalized patients, ribavirin can be considered due to its demonstrated effects in vitro, and from case report-level evidence supporting its use in subacute sclerosing panencephalitis. However, ribavirin is only available under the auspices of an emergency investigational new drug (eIND) application, and not a consideration for use in the emergency department.
Secondary bacterial infections in a patient already suffering from measles should be treated when identified, but prophylaxis is not appropriate. A 2013 Cochrane review noted beneficial effects seen in acute measles patients treated with antibiotics, but cautioned that the vast majority of included randomized controlled trials published between 1939 and 1967. Treatment regimens that include clarithromycin or inhaled budesonide have no evidence backing their utility and should not be used.
The other acute consideration for the emergency department following identification of measles is a determination of whether any post-exposure prophylaxis (PEP) is indicated. Older adults are typically considered immune to measles as a result of exposure prior to eradication of the virus. In the United States, that includes all adults born before 1957, but may include younger adults in other countries. Otherwise, the vast majority of children and adults will be immune due to having received two doses of a measles-containing vaccine.
The mainstays of post-exposure prophylaxis in patients not immune to measles are immune globulin and the measles-mumps-rubella (MMR) vaccine. For infants younger than 6 months, the recommended post-exposure prophylaxis is intramuscular immune globulin at 0.5 mL/kg (maximum dose 15 mL).
For older infants and children, if treated within 72 hours of exposure, the MMR vaccine can be administered. If the exposure history falls into the four- to-six-day window, older infants can be considered for immune globulin, but children typically are not. Once a child or adult has received their first dose of MMR, they do not need to quarantine. In contrast, those who are not immune or have received immune globulin should be instructed to quarantine. Recommended quarantine duration is 21 days from exposure in those who have not received immune globulin, and 28 days in those who do. Edge cases occur in children and adults who have had only one dose of the vaccine, and specific management can be found with the AAP or CDC.
Severely immunocompromised and non-immune pregnant patients present a slightly different pathway for PEP. These patients require a dose of intravenous immune globulin (400 mg/kg of body weight), rather than intramuscular dosing. The immunocompromised and non-immune pregnant patients can receive PEP if treated within 6 days of exposure. The MMR vaccine is not provided to these patients as part of their acute treatment.
The return of measles and other vaccine-preventable illnesses represents avoidable suffering and risk in the emergency department. Regardless, treatment considerations for the affected individual are not complex and primarily supportive. Despite enthusiasm for aspirational alternatives, unproven therapies are more likely to be harmful than beneficial. Long-standing trusted reference sources should take precedence over those of more recent provenance.
 Dr. Radecki (@emlitofnote) is an emergency physician and informatician with Christchurch Hospital in Christchurch, New Zealand. He is the Annals of Emergency Medicine podcast co-host and Journal Club editor.
Dr. Radecki (@emlitofnote) is an emergency physician and informatician with Christchurch Hospital in Christchurch, New Zealand. He is the Annals of Emergency Medicine podcast co-host and Journal Club editor.
References
- Guerra FM, Bolotin S, Lim G, et al. The basic reproduction number (R0) of measles: a systematic review. Lancet Infect Dis. 2017;17(12):e420-e428.
- Ward J, Gressani O, Kim S, Hens N, Edmunds WJ. The epidemiology of pathogens with pandemic potential: A review of key parameters and clustering analysis. Epidemics. 2025;54:100882.
- Sudfeld CR, Navar AM, Halsey NA. Effectiveness of measles vaccination and vitamin A treatment. International Journal of Epidemiology. 2010;39(Supplement 1):i48-i55.
- Kimberlin DW, Banerjee R, Barnett ED, Lynfield R, Sawyer MH, eds. Measles. In: Red Book: 2024–2027 Report of the Committee on Infectious Diseases. 33rd ed. American Academy of Pediatrics345 Park Blvd, Itasca, IL 60143; 2024:570-585.
- Measles (Rubeola). United States Center for Disease Control. https://www.cdc.gov/measles/index.html Accessed 2 Feb 2026.
- Oldham MM, Benavides S, Boylan PM. Navigating measles treatment in 2025: a review on vaccines, medications, and supplements. Pediatr Allergy Immunol Pulmonol. 2025;38(4):113-118.
- Kabra SK, Lodha R. Antibiotics for preventing complications in children with measles. Cochrane Database Syst Rev. 2013;2013(8):CD001477.




No Responses to ““I Found Measles: Now What?””