Procedure

Explore This Issue
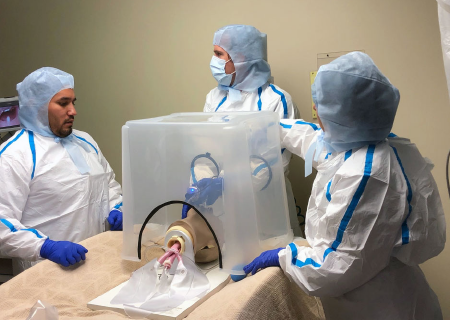
ACEP Now: Vol 39 – No 05 – May 2020Figure 2: Simulated COVID-19 intubation process with protective intubation box.
PHOTOS: David Weech & John Ashurst
Rapid sequence induction medications are administered. The physician then utilizes the two holes to intubate the patient as routinely done (see Figure 2). Once the tube is placed, the stylet is removed and the tube is then clamped with the large forceps, followed by insufflation of the cuff. The options at this point are to remove the intubation box completely as the system is closed or to proceed with the box in place. If the box is kept in place, the nurse passes the ventilator tubing through the caudal aspect of the box and holds the tube in place while a respiratory therapist works through the two primary operator holes to attach the endotracheal tube securing device.
The intubation team then stays in the room for one complete cycle of ambient air, according to local specifications. All necessary related procedures likely to be needed in the near future should be performed at this time to preserve PPE. These may include placement of nasogastric tubes, central lines, arterial lines, chest tubes, etc. The team then moves to the anteroom to doff PPE. This process should be done in a systematic manner: Remove of Tyvek gown and first set of gloves; perform hand hygiene with hand sanitizer; remove the white coverall, boot cover, and second pair of gloves; hand hygiene; place a new set of gloves to remove head covers (including N95); remove of the final pair of gloves; and hand hygiene for a third time. The team may then return to regular duties in the department. Once the patient is transported out of the emergency department, the drapes on the intubation box are discarded. The box is then wiped down with appropriate disinfectant to be reused after the time frame specified by the manufacturer of the disinfectant.
Conclusion
While this rigorous process may seem excessive, we suggest it out of recognition of the severity of the situation we face today. The possibility of losing critical health care workers and medical personnel if they are inadvertently or carelessly exposed to SARS-CoV-2 is far too great to ignore. Emergency departments are among the most critical resources of the health care system. If proper protective measures such as those suggested here are not taken, our ability to save the most lives and to keep the largest number of people healthy will be compromised.
Pages: 1 2 3 | Single Page





No Responses to “How to Intubate Suspected COVID-19 Patients With a Protective Box”